- Center on Health Equity and Access
- Clinical
- Health Care Cost
- Health Care Delivery
- Insurance
- Policy
- Technology
- Value-Based Care
Robotic Lobectomy Techniques Yield Comparable Outcomes in NSCLC
Investigators were searching for answers to the question, “Does it matter if a vein- or artery-first approach is used when performing a robotic lobectomy for non-small cell lung cancer (NSCLC)?
Overall survival (OS) and cancer recurrence did not significantly differ between 2 methods of robotic lobectomy for non-small cell lung cancer (NSCLC), a vein-first technique (V-first) or an artery-first technique (A-first), according to the results from investigators published in Journal of Thoracic Disease.1
This retrospective review was an analysis of electronic medical record data on 2 cohorts of patients (N = 374). Each cohort comprised patients who underwent a robotic lobectomy between January 2013 and May 2019 at the University of Alabama at Birmingham. The patients were sorted by technique used: V-first (n = 94) or A-first (n = 280). Data on postop complications, length of stay (LOS), recurrence-free survival, and OS were collected. More patients in the A-first group had additional work done after their lobectomy vs the V-first group. Thirty-seven percent had an additional artery divided after the vein vs 2% of the V-first group who had an additional vein divided after the artery.
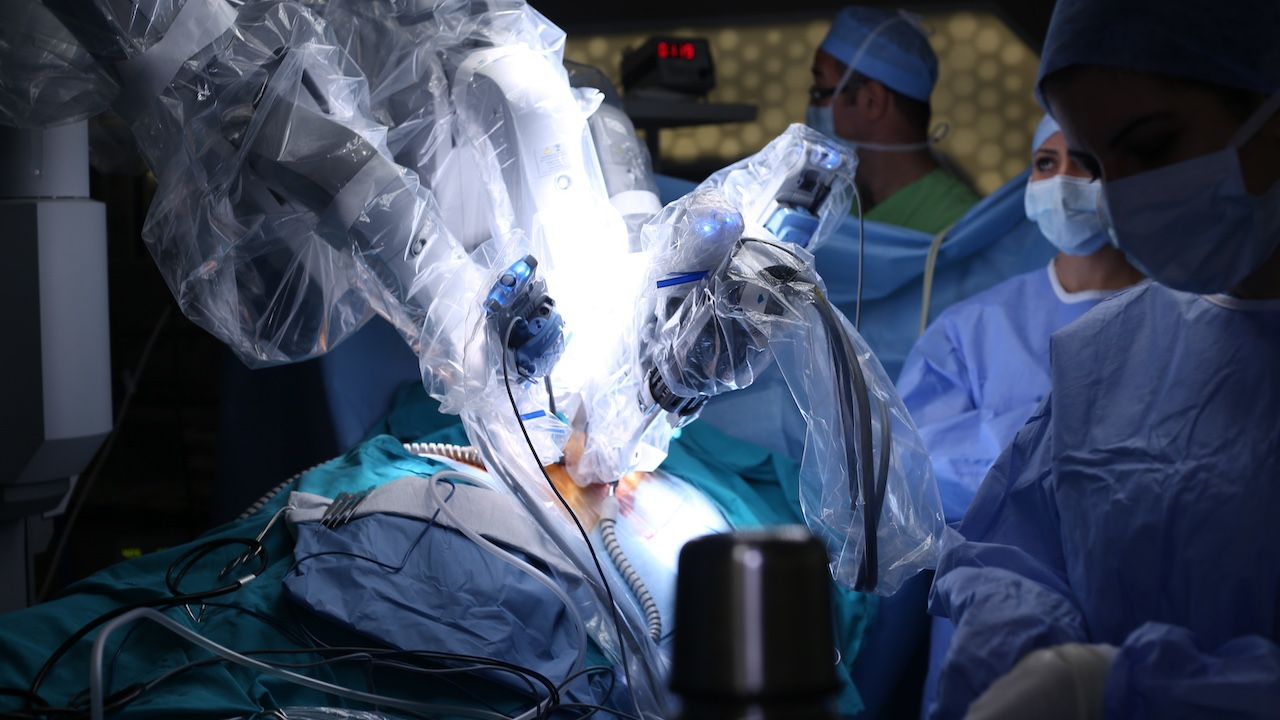
Robotic surgery | Image Credit: Master Video - stock.adobe.com
“Circulating tumor cells can serve as a biomarker for prospective recurrence, making a technique that limits the circulation of these cells an important area of investigation,” the authors wrote. “However, there is little evidence to guide whether a V-first approach to lobectomies is superior to an A-first approach.”
Most of the patients in this analysis were aged 65 to 79 years (54.81%), female patients (58.02%), and Caucasian (84.49%) or Black/African American (14.71%); 53.74% were former smokers. At baseline, the 3 most common comorbidities were hypertension (67.11%), obesity (body mass index, > kg/m2; 36.10%), and chronic obstructive pulmonary disease (34.95%); the most common Zubrod score (the precursor to ECOG Performance Status2) was 1 (62.92%); and the most common tumor size was 2 cm or smaller (33.74%).
V-first was the more common technique used among patients with tumors of 2 cm or smaller (50.0% vs 29.2%; P = .007), and patients who underwent this procedure had a lower mean predicted forced expiratory volume in the first second (78% vs 84%; P = .011). Right upper and right middle lobectomies were more common in the V-first group, at 54.3% and 20.2% vs 36.4% (P = .019) and 2.9% (P < .001), respectively, vs the A-first group. However, more nodes were removed from the patients who underwent A-first operations (21 vs 17; P < .001), and these patients also underwent more left upper lobectomies (23.2% vs 2.1%; P < .001).
Significant differences were not seen regarding postop complications, LOS, or 30- and 90-day mortality. However, atrial arrhythmia was much more common in the A-first vs the V-first group (10.0% vs 4.3%), but did not reach statistical significance.
Adenocarcinoma was the most common form of NSCLC, in 65.8% of the overall study population, and of this group, 70.9% were stage 1. Eight patients were lost to follow-up, and from the 366 who were not, 18.0% had disease recurrence and 16.1% died over a median (IQR) postop follow-up of 67 (45-87) months.
Although the authors noted that neither technique proved superior, they did notice that certain techniques appeared to be more common for certain tumor sizes and locations. For example, A-first was more often used in patients undergoing left upper lobectomies and V-first in patients with tumors of 2 cm or smaller located in their right upper and right middle lobes.
“Ultimately, we found no significant difference in recurrence or overall survival among patients who underwent robotic lobectomies with V-first versus A-first techniques for the resection of NSCLC,” the study authors concluded. “This suggests that the order in which the pulmonary vessels are ligated should be up to the discretion of the surgeon.”
Further study is recommended.
References
- Singh G, Abraham PJ, Xie R, Donahue JM, Wei B. Vein-first vs. artery-first robotic lobectomy outcomes in non-small cell lung cancer. J Thorac Dis. 2024;16(1):368-378. doi:10.21037/jtd-22-1576
- Sheidler V. Performance status measures - a little history. NRG Oncology. May 12, 2021. Accessed February 29, 2024. https://www.nrgoncology.org/Home/News/Post/performance-status-measures---a-little-history
Surgery, Chemotherapy Considered Protective Survival Factors in Patients With OC, Liver Metastases
May 21st 2024Surgery and chemotherapy significantly improved both overall survival (OS) and cancer-specific survival (CSS) in patients with liver metastases originating from ovarian cancer (OC), who generally face a poor prognosis with a 5-year survival rate of less than 30%.
Read More
Frameworks for Advancing Health Equity: Urban Health Outreach
May 9th 2024In the series debut episode of "Frameworks for Advancing Health Equity," Mary Sligh, CRNP, and Chelsea Chappars, of Allegheny Health Network, explain how the Urban Health Outreach program aims to improve health equity for individuals experiencing homelessness.
Listen
Unique Case: HCC With No Cirrhosis—and “Hidden” CLL/SLL
May 21st 2024A 77-year-old man had no risk factors for hepatocellular carcinoma (HCC), but he was nonetheless found to have it. Along the way, he was also diagnosed with previously undetected chronic lymphocytic leukemia/small lymphocytic lymphoma (CLL/SLL).
Read More
