News
Article
Patients With Actinic Keratosis Prefer Simulated Daylight PDT Over More Painful Red Light PDT
Author(s):
A recent study found that patients with actinic keratosis experienced more pain during red light photodynamic therapy (PDT) than simulated daylight PDT, emphasizing the need to understand patient experiences for better treatment decisions.
Patients with actinic keratosis reported more intense pain with red light photodynamic therapy (PDT) compared with simulated daylight PDT (SDL-PDT), according to recent study findings. The results highlighted the importance of understanding patient experiences during PDT to enhance patient-provider decision-making during the course of treatment for the skin condition.
Red light therapy | Image credit: Space_Cat - stock.adobe.com
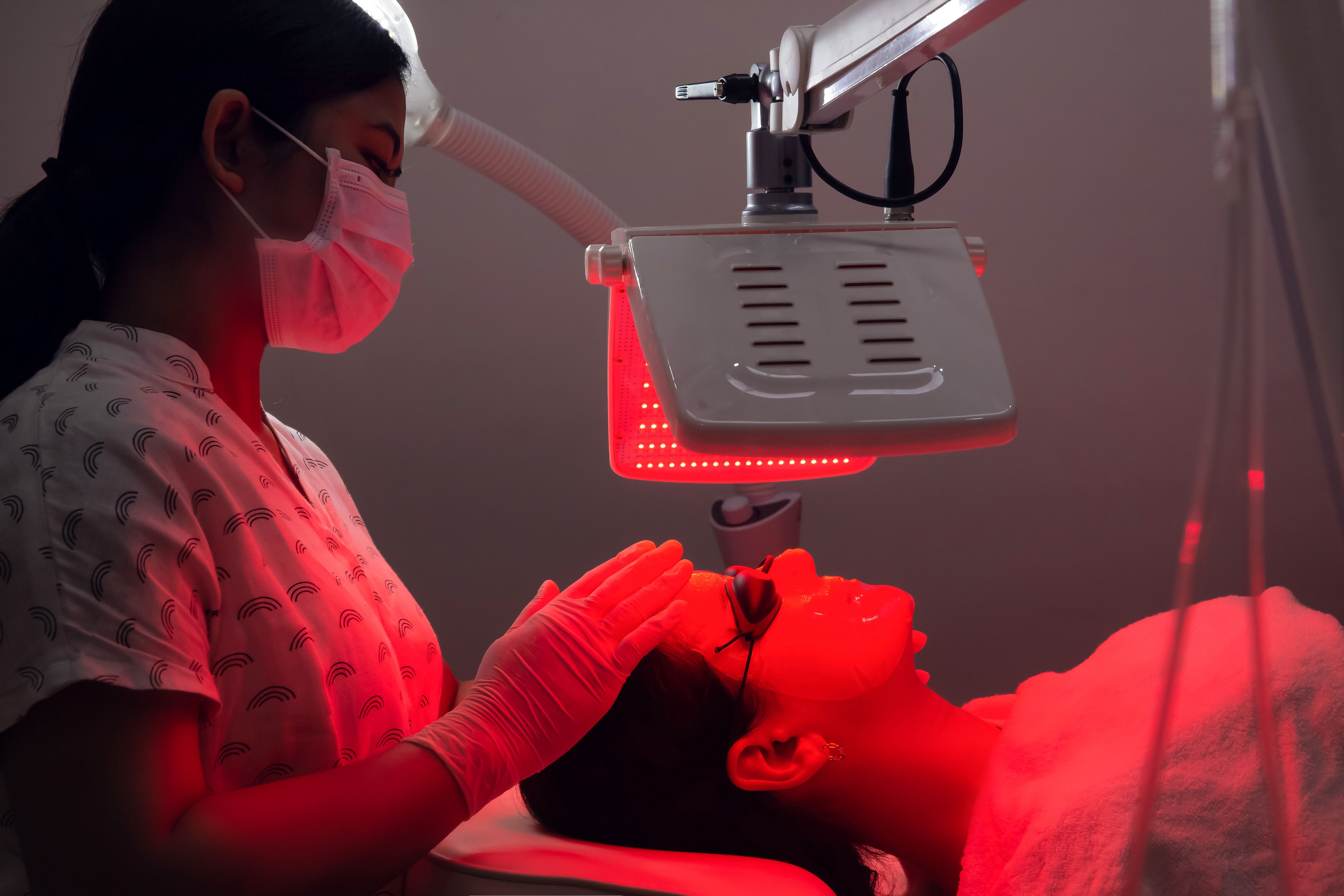
The study, published in Acta Dermato-Venereologica, relied on semistructured interviews to document how patients with actinic keratosis felt about different types of PDT. Compared with conventional red light PDT (C-PDT), SDL-PDT is relatively new and could provide patients with a less painful alternative. However, qualitative research comparing the pain and skin reactions associated with these PDT types is lacking.
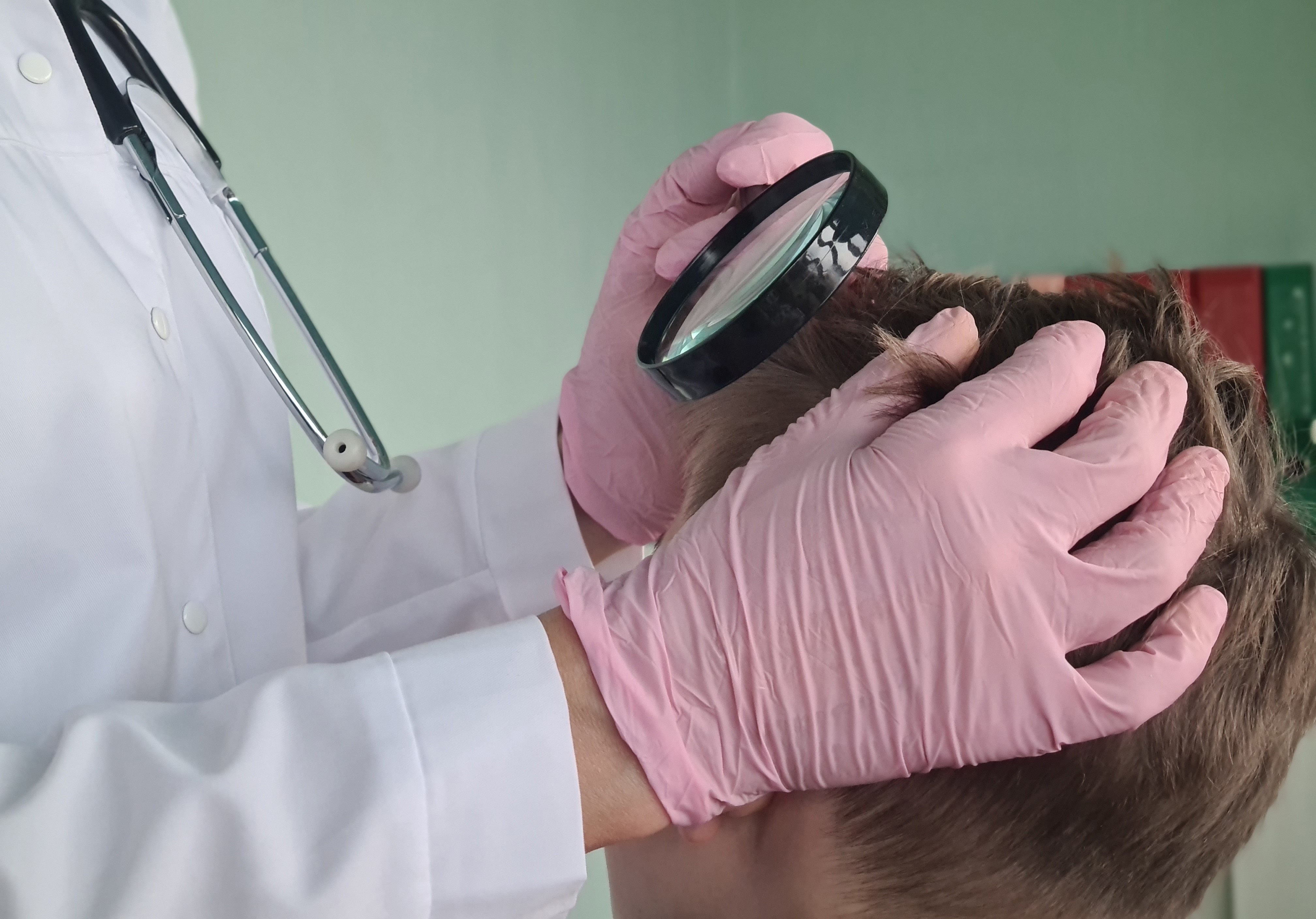
Researchers conducted interviews with 10 patients (male, n = 7) aged 60 to 81 years with symmetrically distributed actinic keratosis. Location of treatment varied from forehead (n = 6), cheeks (n = 4), temples (n = 4), nose (n = 3), scalp (n = 2), forearms (n = 1), and dorsum of the hand (n = 1).
The interviews took place 4 weeks after the patients received split-face treatment with C-PDT and SDL-PDT. The participants were recruited from an ongoing, larger, single-center, randomized controlled trial comparing clinical clearance rates for symmetrically distributed mild to moderate nonpigmented actinic keratosis with PDT. The larger study was conducted at the Department of Dermatology at Sahlgrenska University Hospital in Gothenburg, Sweden.
Duration of the interviewed ranged from 21 to 38 minutes and occurred between June 1, 2022, and January 31, 2023. The researchers categorized the responses into 4 main categories: pain experience, pain management, skin reactions after treatment, and choice of illumination method.
During C-PDT, all patients reported some degree of pain, with describing the sensation as “stinging,” “burning,” or “piercing.” One participant described the pain as if someone had heated up an iron bar and drove it into their forehead. Another described it as “torture,” and some were concerned the pain was so much that they couldn’t make it through the treatment.
Regardless of type of PDT, most patients experienced pain during the first 24 hours after treatment. However, the pain associated with C-PDT persisted during the first week, whereas it diminished quicker with SDL-PDT.
Participants managed pain during C-PDT illumination using mental distraction, short pauses, and water spray, and some prematurely stopped treatment due to pain. In contrast, during SDL-PDT illumination, summarized as “almost painless,” they engaged in pleasant activities like reading or having coffee. After treatment, most followed recommendations to take paracetamol/acetaminophen, while some used cold air, wet towels, cold water rinses, or relied on mental endurance and trust in medical professionals to manage pain.
Regarding skin reactions, the participants noted more intense and longer-lasting skin reactions, including crusting, redness, swelling, and increased scaly and red skin, after C-PDT compared with SDL-PDT. The former also impacted their daily social lives, with some avoiding social contacts post treatment due to soreness and scaling.
Almost all participants (n = 9) indicated that they preferred SDL-PDT over C-PDT. However, several had concerns about the long-term effectiveness of SDL-PDT, which is still unknown. Five participants said that they would prefer 2 treatments with SDL-PDT rather than 1 treatment with C-PDT in the event that SDL-PDT was found to be less effective than C-PDT. One patient indicated they may change their preference depending on which anatomical location was being treated.
The study had some limitations, including that treatment diaries filled out by participants to ensure they accurately recalled their experiences were not analyzed. Additionally, the interviewer was the same health care provider who administered treatment and both PDT methods were performed on the same day, which could make it difficult for the patients to differentiate between the pain during and after treatment.
Reference
Sjöholm A, Claeson M, Paoli J, Heckemann B. Exploring patient pain experiences during and after conventional red light and simulated daylight photodynamic therapy for actinic keratosis: a qualitative interview study. Acta Derm Venereol. Published online April 10, 2024. doi:10.2340/actadv.v104.19459