Supplements and Featured Publications
- Easing the Economic and Clinical Burden of Psoriasis and Psoriatic Arthritis: The Role of Managed Ca
- Volume 22
- Issue 8
Psoriasis and Psoriatic Arthritis Overview
Psoriasis and psoriatic arthritis (PsA) are chronic immune-mediated diseases that primarily affect the skin and joints, respectively; these diseases are also associated with high rates of cardiovascular and other comorbidities. Despite over 40 genes proven to be related to the disease, the exact causes of psoriasis and PsA are still to be determined. Recent insights into the underlying pathophysiology of these diseases have revealed novel therapeutic targets. Effective management requires timely diagnosis and initiation of treatment. Yet, both psoriasis and PsA remain underrecognized and undertreated in current clinical practice. Recognizing the true physical, social, and emotional burden of psoriasis and PsA, as well as their associated comorbidities, is the first step to improving the prognosis for affected patients.
Am J Manag Care. 2016;22:S216-S224
PSORIASIS OVERVIEW
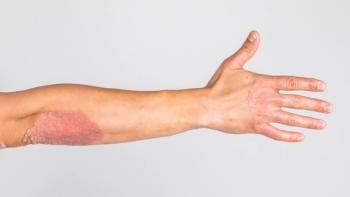
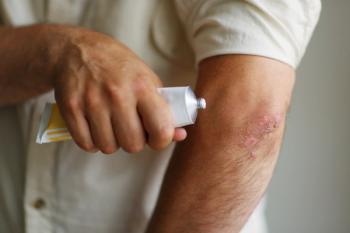
Psoriasis is a chronic, multifactorial, immune-mediated skin disease. The characteristic erythematous plaques of psoriasis are often painful and disfiguring, leading to a substantial decrease in quality of life.1 Cardiovascular disease (CVD), diabetes, and other autoimmune disorders are common among patients with psoriasis, contributing to the overall burden of disease and increasing healthcare
resource utilization.1
Epidemiology
Based on an analysis of National Health and Nutrition Examination Survey data from 2009 to 2010, the estimated prevalence of psoriasis among adults 20 years and older in the United States was 3.2%. The prevalence was highest among Caucasians (3.6%), followed by African Americans (1.9%), Hispanics (1.6%), and others (1.4%). Extrapolating to 2013 US census data, an estimated 7.4 million adults in the United States are living with psoriasis.2
Pathophysiology The precise pathologic mechanisms that drive the development of psoriasis are extremely complex.3 However, recent insights into its pathophysiology have enabled a better understanding of the disease and revealed potential new therapeutic targets.4
Immunologic Mechanisms
Psoriasis is an immune disease that involves abnormally activated cells and molecules of the innate and adaptive immune systems.4 Impaired T-cell activity contributes to the hyperproliferation and abnormal differentiation of epidermal skin cells. Whereas normal epidermal regeneration occurs every 21 to 28 days, the epidermis turns over every 3 to 4 days in patients with psoriasis.3
Keratinocytes, the most predominant type of epidermal cells, are key mediators of impaired immune cell function. In patients with psoriasis, keratinocytes recruit inflammatory dendritic cells to release interleukin (IL)-12 and IL-23, which, in turn, activate T-cells to produce other psoriatic cytokines, such as IL-17, IL-22, interferon (IFN)-gamma, and tumor necrosis factor-α (TNF-α). In
particular, IL-17 and IL-23 appear to be the dominant cytokines driving the aberrant activity of T-cells and keratinocytes in psoriasis. Current and emerging biologic therapies target these two important cytokines, as well as others, to control psoriatic inflammation.4
Genetics of Psoriasis
As a multifactorial disease, psoriasis has a complex genetic basis. Genetic studies have revealed more than 40 loci associated with psoriasis susceptibility, each with multiple genes that are involved in skin barrier functions, as well as innate and adaptive immunity. The involvement of these genes and their encoded proteins supports the central role of altered immune function in the pathogenesis of psoriasis.5
The different clinical phenotypes of psoriasis appear to correspond with distinct immunogenetic profiles.The estimated heritability of psoriasis—a measure that describes how much of the observed phenotypic variation is attributable to genetic variation—is 60% to 90%; this is one of the highest rates among complex genetic diseases. In the future, genetic testing is likely to play an important role in predicting the clinical course of psoriasis, as well as the likelihood of response to specific treatment options.5
Other Risk Factors In addition to genetics and altered immune function, several other risk factors may predispose patients to psoriasis. These include3:
• Environmental triggers (infection, stress)
• Medications (lithium, beta-blockers)
• Other immune-mediated diseases (Crohn’s disease, multiple sclerosis)
• Psychogenic stressors, particularly in pediatric patients (emotional or mental stress)
Presentation and Diagnosis Most patients with psoriasis present without other clinical manifestations. In symptomatic patients, common manifestations include pruritus, fever, and malaise.3 Even in the absence of comorbid psoriatic arthritis (PsA), joint pain is a common presentation in patients with psoriasis. In one study, 51.8% of patients with psoriasis who did not have PsA reported joint pain. Of those with joint pain, 48.1% experienced pain in more than 4 joints.6 The onset of psoriasis can occur at any age; however, new diagnoses tend to follow a bimodal distribution around young adulthood (20-35 years old) and middle age (50-60 years old). Although male and female patients are affected equally across all age groups, younger men tend to be affected more frequently than younger women.3 The diagnosis of psoriasis is often delayed by several years after symptom onset. In one population-based cohort study of US patients with psoriasis (N = 1005), the median age of diagnosis was 37 years, and the median age of symptom onset was 34 years.6
Disease Classification
The major subtypes of psoriasis are based on historic descriptions of its underlying histology and morphology. In the clinical setting, however, patients often present with more than 1 subtype of psoriasis.1
Plaque Psoriasis The most common clinical phenotype is plaque psoriasis, which affects approximately 80% to 90% of patients with this disease (
Pustular Psoriasis
Neutrophils are commonly present in the outermost layer of the skin in patients with psoriatic lesions. When enough neutrophils accumulate to manifest in clinical signs and symptoms, it is classified as pustular psoriasis (
Guttate Psoriasis
Guttate psoriasis affects less than 2% of patients with psoriasis, and it is seen primarily in patients younger than 30 years (
Nail Psoriasis
Patients with any subtype of psoriasis can also exhibit characteristic psoriatic nail changes, such as pitting (partial loss of cells from the surface of the nail plate), onycholysis (separation of the nail from the nail bed), subungual hyperkeratosis (scaling under the nail), and the oil-drop sign (translucent discoloration in the nail bed). Approximately 60% of all patients with psoriasis will experience fingernail changes, and 35% will experience toenail changes. However, nail psoriasis is considered a marker for PsA, particularly in patients with distal interphalangeal joint involvement (
Erythrodermic Psoriasis
Patients with erythrodermic psoriasis present with generalized erythema that covers major portions of the body surface area (BSA). This type of psoriasis can occur suddenly in a patient with little history of the disease or develop gradually from chronic plaques. Erythrodermic skin exhibits altered thermoregulatory properties, leading to a range of potential symptoms, such as hypothermia, chills, dehydration from fluid loss, fever, malaise, lower leg edema, and congestive heart failure (
Inverse Psoriasis
Inverse psoriasis describes psoriatic lesions that occur in the skin folds, such as the axillary, genital, abdominal, perineal, intergluteal, and inframammary areas (
Assessment of Disease Activity
The severity of psoriasis is defined by the areas affected and the percentage of BSA covered. However, psoriasis is classified as severe when lesions affect the hands, feet, face, scalp, or genitals, regardless of the BSA affected. When these areas are not affected, psoriasis is described as:
• Mild (<5% of BSA)
• Moderate (5%-10% of BSA)
• Severe (>10% of BSA)
The majority of patients with psoriasis (70% to 75%) will present with mild to moderate disease.3 Composite measures of disease activity can also be used to assess psoriasis disease severity and monitor the effect of treatment over time.1
Composite Measures of Disease Activity The Psoriasis Area and Severity Index (PASI), the standard tool in psoriasis clinical trials for assessing baseline disease severity and monitoring therapeutic response, is the most common composite tool for measuring psoriasis severity.1 Calculating the total PASI score is a 2-step process. First, clinicians assign a score from 0 (complete lack) to 4 (most severe possible) to describe
the presence and severity of each of 3 components of psoriatic plaques (erythema, induration, and desquamation) within each of 4 regions of the body (head/neck, trunk, upper extremities, and lower extremities). Second, clinicians estimate the extent of skin involvement by assigning a grade from 0 (no psoriasis) to 6 (90%-100% involvement) to estimate the BSA within each of the 4 body regions. Utilizing a complex algorithm, the individual scores are used to calculate a total PASI score that can range from 0 to 72. In real-world clinical practice, PASI scores higher than 36 are rare.8
Critics of the PASI argue that the tool does not correspond well with the patient’s experience of psoriasis severity. The PASI algorithm assigns equal weight to lesions occurring anywhere on the body; however, plaques that affect the face, hands, and anogenital area are considered by patients to be more severe than those located elsewhere.8 Furthermore, the PASI does not capture other aspects of psoriasis that are important to patients. When patients with psoriasis (N = 1005) were asked to rank the top 5 most important factors contributing to disease severity, more than one-third (36.1%) ranked itching as the most important factor. Additional factors included location/size of lesions (21.8%), flaking (11.4%), scaling (8.3%), and pain/swelling of joints (5.4%). Despite being the most important symptom for many patients, itching is not captured in the PASI or other instruments such as the Physician Global Assessment. Therefore, current tools may underestimate the true burden of psoriasis on patients.6
New options for assessing the severity of psoriasis, with an emphasis on patient-reported outcomes, have recently been implemented. These tools facilitate an improved understanding of the impact of psoriasis on patients’ lives, and provide better instruments for measuring the efficacy of powerful new treatments in clinical practice.8
Differential Diagnosis
Not all cases of psoriasis present with characteristic erythematous, scaling, or silvery plaques. When lesions are misleading, the differential diagnosis of psoriasis can be challenging, and it may vary by psoriasis subtype.3 Plaque type psoriasis is often confused with eczema, fungal infections such as tinea corporis, squamous cell carcinoma (Bowen’s disease), cutaneous T-cell lymphoma
(CTCL) and subacute cutaneous lupus erythematous.Pustular psoriasis should be differentiated from candidiasis and acute generalized exanthematic pustulosis. Guttate psoriasis can appear similar to secondary syphilis or pityriasis rosea. Erythrodermic psoriasis should be differentiated from pityriasis rubra pilaris, Sézary syndrome, drug eruptions, and even Norwegian scabies. Finally, inverse
psoriasis can have a similar presentation to intertrigo, candidiasis, or tinea cruris.3
Comorbidities Patients with psoriasis, particularly those who are already burdened with moderate to severe skin disease and those with PsA, face a high risk of comorbidities.9 Approximately 75% of patients with psoriasis have at least 1 comorbid condition.6 A recent analysis of a large US administrative claims database revealed the scope and prevalence of comorbidities in patients with psoriasis. The study compared healthcare utilization patterns among patients with moderate to severe psoriasis (N = 5492) and controls without psoriasis or PsA matched by age, gender, and geographic region (N = 5492). The most common comorbidities in patients with psoriasis were cardiometabolic risk factors such as hyperlipidemia, hypertension, and diabetes. These, as well as multiple other comorbidities including obesity and the metabolic syndrome, occurred with significantly greater frequency among patients with psoriasis than among controls. Hyperlipidemia was present in 33% versus 27%, hypertension in 33% versus 24%, and diabetes in 16% versus 10% of psoriasis versus non-psoriasis patients, respectively; in addition, 22.1% of patients with psoriasis also had a diagnosis of PsA.10
Given their high burden of comorbidities, patients with psoriasis have many interactions with the healthcare system. During the 12-month study period, patients with psoriasis were more likely than individuals without psoriasis to have any prescription medications filled (98.8% vs 76.6%; odds ratio [OR], 27.5; P <.001) and had a higher number of distinct medications filled (10.9 vs 5.2; incident
rate ratio [IRR], 2.1; P <.001). In addition to utilizing a range of psoriasis treatments, including biologic therapy (65.2%), nonbiologic systemic therapy (27.3%), and phototherapy (16.5%), patients with psoriasis were more likely than controls to fill prescriptions for antidepressants (25% vs 13.9%; OR, 2.1; P <.001), antidiabetic drugs (11.3% vs 6.8%; OR, 1.7%; P <.001), and cardiovascular drugs (47.9% vs 36.1%; OR, 1.7%; P <.001). Furthermore, patients with psoriasis were significantly more likely than non-psoriasis controls to utilize medical services during the 12-month observational period. This included a higher likelihood of outpatient visits (99.0% vs 84.5%; OR, 29.3; P < .001), emergency department visits (21.4% vs 16.4%; OR, 1.3; P <.001), and hospital admissions (9.3% vs 6.4%; OR, 1.3; P = .001).10 These findings highlight the economic implications of comorbidity management in patents with psoriasis.
Patient Expectations
In addition to having medical comorbidities, patients with psoriasis may experience a range of profound psychosocial and behavioral challenges throughout the course of their disease. Each life stage is associated with a different mix of predominant concerns from the patient’s perspective (
Quality of Life
Across the lifespan, quality of life is of particular concern. Patients with moderate to severe psoriasis commonly report negative social, emotional, and other life experiences that they attribute to their disease. Suicidal ideation is significantly increased in younger psoriasis patients.
Treatment
Psoriasis management has undergone a major paradigm shift from older therapies to newer biologic agents. With this change in focus, managed care organizations face new challenges in balancing the benefits, limitations, and pharmacoeconomics of current and emerging therapies. See Part 2 of this continuing education supplement for a review of current local and systemic options for psoriasis treatment.
PSORIATIC ARTHRITIS OVERVIEW
PsA is an underdiagnosed and undertreated inflammatory joint disease that develops in a substantial minority of patients with psoriasis. Although the clinical course is variable, many patients with PsA can experience progressive joint disease, impaired physical function, and decreased quality of life.13
Prevalence and Epidemiology
Among patients with psoriasis, the prevalence of PsA in recent US cohort studies ranged from 22% to 27%.6,10 Overall, PsA affects approximately 0.1% to 0.2% of the general population.14 The clinical manifestations of PsA tend to emerge 5-12 years after initial skin presentation (ie, between the ages of 30 and 50 years in affected individuals). As with psoriasis, men and women are equally likely to develop PsA.15
Pathophysiology Although the etiology of PsA remains still to be completely understood, multiple immune system cell types and cytokines have been implicated in PsA disease activity.14,15 The synovial fluid of joints affected by PsA shows increased levels of T-cells and cytokines such as TNF, IL-6, IL-12/IL-23, and IL-17.15 Together, these cytokines drive joint inflammation and other downstream biological effects, such as osteoblast and osteoclast activation, which further contributes to joint damage.16 Biologic therapies targeting these aberrant signaling pathways have emerged as key treatment options for PsA, particularly for patients with moderate to severe disease.13
Presentation and Prognosis
The classic clinical manifestations of PsA include swelling, tenderness, stiffness, and pain of the joints and surrounding tissues.15 Dactylitis (“sausage digit”) is a hallmark feature of PsA that involves swelling of the joints, tendons, ligaments, and synovial tissue in the hands and/or feet (
The clinical course of PsA is characterized by a series of remissions and disease flares, with fewer than 20% of patients experiencing prolonged remissions.13 Prognosis is unpredictable and varies from mild joint disease to severe and debilitating outcomes.15 Approximately 25% to 30% of patients will experience relatively benign joint inflammation, with limited disability over time. For up to 60% of patients, however, PsA is associated with progressive, erosive, and deforming joint damage. Severely deforming arthritis (arthritis mutilans) affects approximately 5% of patients with PsA.17
One of the major barriers to improved prognosis involves widespread undertreatment.6 Many patients with PsA do not receive the recommended systemic therapies to slow disease progression.13 In the Multinational Assessment of Psoriasis and Psoriatic Arthritis (MAPP) survey (N = 1005), only half of patients were being treated with conventional oral therapy (24%) or biologic therapy (26%) to address their joint symptoms.6 Without recommended treatment, a significant portion of patients with PsA will experience ongoing systemic inflammation, progressive joint damage, severe disability, multiple comorbidities, and increased mortality.15,18-20
Diagnosis
The diagnosis of PsA is made on the basis of the modified Classification Criteria for Psoriatic Arthritis (CASPAR).13,21 To confirm a diagnosis of PsA, a patient with musculoskeletal symptoms, such as arthritis, enthesitis, and/or spondylitis, must score at least 3 points using the CASPAR criteria (
To achieve tight control of disease activity to improve joint outcomes, early detection of PsA is critical for initiating appropriate treatment.22 However, making a timely diagnosis of PsA is challenging across provider specialties. In the MAPP survey, 37.6% of dermatologists (N = 101) described differentiating PsA from other arthritic diseases as the greatest challenge in managing patients with PsA. In addition, 25.0% of rheumatologists (N = 100) cited delayed referral of patients as one of the greatest challenges in managing the population of patients with PsA. Furthermore, the majority of dermatologists (87.1%) and rheumatologists (85.0%) indicated that, because of the failure to make the connection between skin and joint symptoms, PsA is likely underdiagnosed in patients with psoriasis.6 Indeed, one recent meta-analysis found that the prevalence of undiagnosed PsA among patients with psoriasis (N = 7831) was 15.5%.22 To minimize the delay in diagnosing PsA, dermatologists are encouraged to screen patients with psoriasis for the signs and symptoms of PsA at every clinic visit.13,15 Screening questionnaires are useful tools for detecting rheumatologic symptoms in patients with psoriasis.22 The Psoriasis and Arthritis Screening Questionnaire, Psoriasis Epidemiology Screening Tool, and Toronto Psoriatic
Arthritis Screen can be used by dermatologists and other providers to identify patients with potential PsA who require further assessment by a rheumatologist.22,23
Differential Diagnosis
The differential diagnoses of PsA include rheumatoid arthritis, erosive osteoarthritis, crystal arthritis (eg, gout and pseudogout), and other seronegative spondyloarthropathies, such as reactive arthritis, enteropathic arthritis, and ankylosing spondylitis.14
Comorbidities
More than half of patients with PsA will have at least 1 comorbidity that contributes to the patient’s overall disease burden.18 It is not uncommon to diagnose multiple medical comorbidities in this patient population. In a study of 631 patients with PsA, 42% had 3 or more comorbid conditions.24
Cardiovascular comorbidities are of particular concern for patients with PsA, given the high morbidity and mortality burden of CVD.19,20 One large population cohort study examined the incidence of CVD and major adverse cardiovascular events (MACE; defined as myocardial infarction [MI], stroke, or sudden death) in both patients with PsA (N = 7982) and in those without PsA (N = 74,583). For this analysis, CVD was defined as any diagnosis of arrhythmia, ischemic heart disease, angina, MI, stroke, pericardial disease, pulmonary hypertension, or sudden death. The rate of incident CVD was 12.8 cases per 1000 person-years among patients with PsA, or 33% higher than the rate of 9.6 cases per 1000 person-years in individuals without PsA (IRR, 1.33; 95% CI, 1.23-1.44). Patients with PsA also had a significantly higher rate of MACE. The MACE rate was 4.6 events per 1000 personyears in the PsA group and 3.5 events per 1000 personyears in the non-PsA group (IRR, 1.30; 95% CI, 1.15-1.47). Together, these findings support the association between PsA and increased risk of CVD and MACE.19
Another recent population-based longitudinal cohort study examined the risk of MACE in patients with PsA (N = 8706), psoriasis (N = 138,424), or rheumatoid arthritis (N = 41,742) and in unaffected individuals (N = 81,573). After controlling for traditional cardiovascular risk factors, patients with PsA who were not undergoing treatment with disease-modifying antirheumatic drugs (DMARDs) were 24% more likely to experience MACE than were controls (hazard ratio [HR], 1.24; 95% CI, 1.03-1.49). By comparison, patients with PsA who were treated with DMARDs did not have a significantly increased risk of MACE (HR, 1.17; 95% CI, 0.95-1.46). These findings highlight the importance of appropriate treatment to control underlying disease activity and address excess cardiovascular risk.20 Additional comorbid conditions in patients with PsA can include osteoporosis, autoimmune ophthalmic diseases (uveitis), liver disease, inflammatory bowel disease, kidney disease, malignancy, and infection.18
Patient Expectations The burden of PsA and its treatment can adversely affect quality of life for many patients.6 Depression and anxiety are highly prevalent among patients with PsA, particularly among those with more severe disease.18 Dissatisfaction with various aspects of PsA disease management—including treatment efficacy and tolerability, monitoring requirements, and convenience—is common.25 Importantly, patients with PsA may assess disease severity differently from providers, underscoring the need for open patient-provider communication to ensure that the patient’s treatment priorities are being addressed.6
The burden of PsA and its treatment can adversely affect quality of life for many patients.6 Depression and anxiety are highly prevalent among patients with PsA, particularly among those with more severe disease.18 Dissatisfaction with various aspects of PsA disease management—including treatment efficacy and tolerability, monitoring requirements, and convenience—is common.25 Importantly, patients with PsA may assess disease severity differently from providers, underscoring the need for open patient-provider communication to ensure that the patient’s treatment priorities are being addressed.6
Treatment The goals of treatment in PsA are to control inflammatory disease activity, manage joint pain, improve mobility, safeguard patient quality of life, and prevent joint destruction. Given that focusing on the skin disease alone will not improve joint symptoms in PsA, patient management ideally involves a multidisciplinary collaboration with input from dermatology and rheumatology. With the development of novel biologic therapies, clinicians have new options for targeting the underlying pathophysiology of PsA.13 See part 2 for a detailed overview of current and emerging PsA treatment strategies.
CONCLUSION
Psoriasis and PsA are chronic immune-mediated diseases with high rates of cardiovascular and other comorbidities. Recent insights into the underlying pathophysiology of these diseases have revealed novel therapeutic targets. The diseases are underrecognized and undertreated in current clinical practice. Recognizing the true burdens of psoriasis and PsA and their common comorbidities is the first step to improving the prognosis for affected patients.
Author affiliation: Baylor University Medical Center, Dallas, Texas.
Funding source: This activity is supported by educational grants from Lilly and Novartis.
Author disclosure: Dr Menter has no relevant financial relationships with commercial interests to disclose.
Authorship information: Concept and design, drafting of the manuscript, and critical revision of the manuscript for important intellectual content.
Address correspondence to: amderm@gmail.com.
1. Menter A, Gottlieb A, Feldman SR, et al. Guidelines of care for the management of psoriasis and psoriatic arthritis: section 1. Overview of psoriasis and guidelines of care for the treatment
of psoriasis with biologics. J Am Acad Dermatol. 2008;58(5):826-850. doi: 10.1016/j.jaad.2008.02.039.
2. Rachakonda TD, Schupp CW, Armstrong AW. Psoriasis prevalence among adults in the United States. J Am Acad Dermatol. 2014;70(3):512-516. doi: 10.1016/j.jaad.2013.11.013.
3. Nguyen TT. Papulosquamous eruptions. In: Bope ET, Killerman RD, eds. Conn’s Current Therapy 2016. Philadelphia, PA: Elsevier, Inc; 2016:275-280.
4. Kim J, Krueger JG. The immunopathogenesis of psoriasis. Dermatol Clin. 2015;33(1):13-23. doi: 10.1016/j.det.2014.09.002.
5. Mahil SK, Capon F, Barker JN. Genetics of psoriasis. Dermatol Clin. 2015;33(1):1-11. doi: 10.1016/j.det.2014.09.001.
6. Lebwohl MG, Kavanaugh A, Armstrong AW, Van Voorhees AS. US perspectives in the management of psoriasis and psoriatic arthritis: patient and physician results from the population-based
Multinational Assessment of Psoriasis and Psoriatic Arthritis (MAPP) Survey. Am J Clin Dermatol. 2016;17(1):87-97. doi:10.1007/s40257-015-0169-x.
8. Chalmers RJ. Assessing psoriasis severity and outcomes for clinical trials and routine clinical practice. Dermatol Clin. 2015;33(1):57-71. doi: 10.1016/j.det.2014.09.005.
9. Ryan C, Kirby B. Psoriasis is a systemic disease with multiple cardiovascular and metabolic comorbidities. Dermatol Clin. 2015;33(1):41-55. doi: 10.1016/j.det.2014.09.004.
10. Feldman SR, Zhao Y, Shi L, Tran MH, Lu J. Economic and comorbidity burden among moderate-to-severe psoriasis patients with comorbid psoriatic arthritis. Arthritis Care Res (Hoboken). 2015;67(5):708-717. doi: 10.1002/acr.22492.
11. Garshick MK, Kimball AB. Psoriasis and the life cycle of persistent life effects. Dermatol Clin. 2015;33(1):25-39. doi: 10.1016/j.det.2014.09.003.
12. Pariser D, Schenkel B, Carter C, Farahi K, Brown TM, Ellis CN; Psoriasis Patient Interview Study Group. A multicenter, noninterventional study to evaluate patient-reported experiences of
living with psoriasis. J Dermatolog Treat. 2016;27(1):19-26. doi:10.3109/09546634.2015.1044492.
7. Ryan C, Sadlier M, De Vol E, et al. Genital psoriasis is associated with significant impairment in quality of life and sexual functioning. J Am Acad Dermatol. 2015;72(6):978-83. doi: 10.1016/j.jaad.2015.02.1127.
13. Tintle SJ, Gottlieb AB. Psoriatic arthritis for the dermatologist. Dermatol Clin. 2015;33(1):127-148. doi: 10.1016/j.det.2014.09.010.
14. Ferri FF. Psoriatic arthritis. In: Ferri FF, ed. Ferri’s Clinical Advisor 2016. Philadelphia, PA: Elsevier, Inc; 2016:1040-1041.
15. Gottlieb A, Korman NJ, Gordon KB, et al. Guidelines of care for the management of psoriasis and psoriatic arthritis: section 2. Psoriatic arthritis: overview and guidelines of care for treatment
with an emphasis on the biologics. J Am Acad Dermatol. 2008;58(5):851-864. doi: 10.1016/j.jaad.2008.02.040.
16. Adamopoulos IE, Pflanz S. The emerging role of interleukin 27 in inflammatory arthritis and bone destruction. Cytokine Growth Factor Rev. 2013;24(2):115-121. doi: 10.1016/j.cytogfr.2012.10.001
17. Helliwell PS, Ruderman EM. Natural history, prognosis, and socioeconomic aspects of psoriatic arthritis. Rheum Dis Clin North Am. 2015;41(4):581-591. doi: 10.1016/j.rdc.2015.07.004.
18. Husni ME. Comorbidities in psoriatic arthritis. Rheum Dis Clin North Am. 2015;41(4):677-698. doi: 10.1016/j.rdc.2015.07.008.
19. Li L, Hagberg KW, Peng M, Shah K, Paris M, Jick S. Rates of cardiovascular disease and major adverse cardiovascular events in patients with psoriatic arthritis compared to patients without
psoriatic arthritis. J Clin Rheumatol. 2015;21(8):405-410. doi:10.1097/RHU.0000000000000306.
20. Ogdie A, Yu Y, Haynes K, et al. Risk of major cardiovascular events in patients with psoriatic arthritis, psoriasis and rheumatoid arthritis: a population-based cohort study. Ann Rheum Dis. 2015;74(2):326-332. doi: 10.1136/annrheumdis-2014-205675.
21. Taylor W, Gladman D, Helliwell P, Marchesoni A, Mease P, Mielants H; CASPAR Study Group. Classification criteria for psoriatic arthritis: development of new criteria from a large international
study. Arthritis Rheum. 2006;54(8):2665-2673.
22. Villani AP, Rouzaud M, Sevrain M, et al. Prevalence of undiagnosed psoriatic arthritis among psoriasis patients: systematic review and meta-analysis. J Am Acad Dermatol. 2015;73(2):242-
248. doi: 10.1016/j.jaad.2015.05.001.
23. Mease PJ, Gladman DD, Helliwell P, et al. Comparative performance of psoriatic arthritis screening tools in patients with psoriasis in European/North American dermatology clinics. J Am Acad Dermatol. 2014;71(4):649-655. doi: 10.1016/j.jaad.2014.05.010.
24. Husted JA, Thavaneswaran A, Chandran V, Gladman DD.
Incremental effects of comorbidity on quality of life in patients with psoriatic arthritis. J Rheumatol. 2013;40(8):1349-1356. doi:10.3899/jrheum.121500.
25. Armstrong AW, Robertson AD, Wu J, Schupp C, Lebwohl MG. Undertreatment, treatment trends, and treatment dissatisfaction among patients with psoriasis and psoriatic arthritis in the United States: findings from the National Psoriasis Foundation surveys, 2003-2011. JAMA Dermatol. 2013;149(10):1180-1185. doi:10.1001/jamadermatol.2013.5264.
Articles in this issue
over 9 years ago
Managed Care Aspects of Psoriasis and Psoriatic Arthritisover 9 years ago
Psoriasis and Psoriatic Arthritis TreatmentNewsletter
Stay ahead of policy, cost, and value—subscribe to AJMC for expert insights at the intersection of clinical care and health economics.