Video
Definition, Diagnosis, and Progression of Psoriasis
Joel Gelfand, MD, MSCE, FAAD; Peter Dehnel, MD; and Steven Feldman, MD, PhD, provide an overview of psoriasis, including diagnosis, genetic influence, and progression.
Transcript
Peter L. Salgo, MD: Psoriasis is a chronic systemic inflammatory disease that targets the skin and the joints. It has been reported that psoriasis increases the risk of developing metabolic syndrome, including obesity, dyslipidemia, diabetes, and hypertension.
Well, we’ve got a panel of experts today to provide an understanding of these comorbid conditions and discuss the causal relationship between the 2 conditions among other things. We’re also going to dive deeper into the biologics used to treat psoriasis and review their efficacy in patients who also present with metabolic syndrome.
I am Dr Peter Salgo. I’m a professor of medicine and anesthesiology at Columbia University Vagelos College of Physicians and Surgeons and associate director of surgical intensive care at NewYork-Presbyterian Hospital in New York City.
Joining me today are Dr Joel Gelfand, professor of dermatology and epidemiology, vice chair of clinical research, and medical director in the Dermatology Clinical Studies Unit, and director of the Psoriasis and Phototherapy Treatment Center at the University of Pennsylvania Perelman School of Medicine in Philadelphia, Pennsylvania;
Dr Peter Dehnel, currently a medical director, and he’s also held multiple previous positions, with Blue Cross affiliates in the North Central United States;
And Dr Steven Feldman, professor of dermatology at Wake Forest School of Medicine in Winston-Salem, North Carolina.
Thank you all so much for being here. It’s a pleasure to be on the same panel with you. Why don’t we start with the basic stuff. I’ll ask the obvious question: what is psoriasis? Anybody want to jump in on that?
Steven Feldman, MD, PhD: Oh, with pleasure.
Peter L. Salgo, MD: I knew you would.
Steven Feldman, MD, PhD: Psoriasis is an immune disease. It causes red, scaly lesions of the skin. I’ve been caring for patients with psoriasis for over 25 years now, and I don’t have a really great definition for it. Like with diabetes, you don’t have enough insulin action. With psoriasis…you know it when you see it, and that’s often how we define it in clinical studies. A dermatologist says, that’s psoriasis.
Peter L. Salgo, MD: You know, back even in the 1960s when I was a kid I remember this TV commercial talking about the “heartbreak of psoriasis,” and even then it was, you know it when you see it. Did you ever see that commercial?
Joel Gelfand, MD, MSCE, FAAD: I’m very much aware of it, and times have not changed that much. I think that despite all the progress we’ve made in psoriasis care, understanding how the disease works, there’s still a lot of stigma associated with this disease. We recently published a paper surveying people in the United States, and roughly a third of people think that psoriasis is contagious, would not want to shake hands with someone who has visible psoriasis, things of that nature. Our patients face a lot of burden and stigma in society trying to deal with this chronic disease.
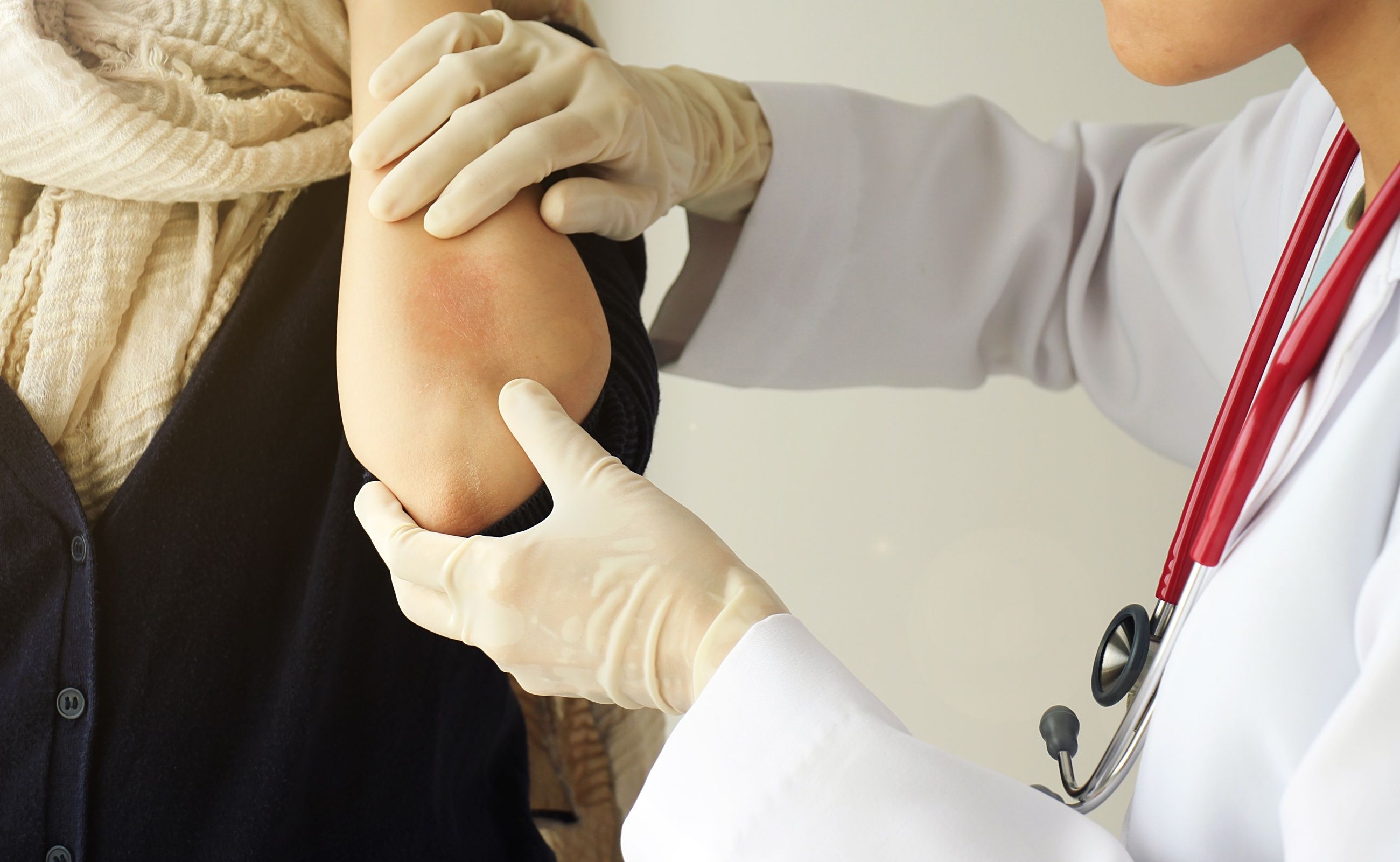
Peter L. Salgo, MD: I think the lay public believes that it’s usually just your elbows and that’s it, some sort of skin disease. Nothing could be further from the truth, right?
Steven Feldman, MD, PhD: Right. It can affect the scalp, not commonly the face but it could be on the face, the elbows as you point out, the nails, the knees, the belly button, at the lower portion of the back.
Peter L. Salgo, MD: I love dermatologists. They’re just great.
Steven Feldman, MD, PhD: It can be all over or it could just be limited areas. Genital involvement is another common area people don’t talk about.
Peter L. Salgo, MD: If you can’t catch it, how do you get it? Is it genetic? Do you inherit a tendency to get this disease?
Joel Gelfand, MD, MSCE, FAAD: Of all the complex genetic traits, psoriasis is probably one of the most heritable. Think about things like type 2 diabetes, or Crohn’s disease, or multiple sclerosis, out of all those, psoriasis has the strongest genetic component to it out of these complex multigenic diseases. About 40% of people who have psoriasis will have a family history of psoriasis as well, and that’s important for people to be aware of. Oftentimes, people worry about will their children develop psoriasis, and it’s about a 20% lifetime risk of someone who has psoriasis passing it on to their children.
Peter L. Salgo, MD: That’s a fairly significant risk.
Joel Gelfand, MD, MSCE, FAAD: It is.
Peter L. Salgo, MD: Frankly.
Joel Gelfand, MD, MSCE, FAAD: Yes.
Peter L. Salgo, MD: How does it progress? Does it start with 1 plaque, 1 lesion, and then spread or is it multicentric often from the beginning? What’s the clinical progression of this thing?
Joel Gelfand, MD, MSCE, FAAD: It’s so variable, that’s what’s so difficult for patients. It’s often hard to know who’s going to have fairly limited disease that will stay limited for their life. And this is a disease that could start at any stage of life. It could start in infancy or late adolescence, in the early 20s. I’ve had a patient develop psoriasis when she was in her mid-80s when her sister died, so oftentimes as major stressful life event can bring it on.
Peter L. Salgo, MD: I was going to say, I’ve heard that from patients. Everything was great and then something big happened in my life and then everything exploded.
Joel Gelfand, MD, MSCE, FAAD: Yes, and we know with genetic susceptibility that people are prone to having their immune system recognize proteins that are made by the skin, by the keratinocytes and melanocytes that are completely normal, and then the body reacts in an autoimmune fashion to those proteins.
Peter L. Salgo, MD: OK.
Steven Feldman, MD, PhD: Peter, there’s a lot of dogma about progression, and I think it’s a very hard thing to study. Joel, you’ve done some great work on progression in eczema showing that the dogma doesn’t really fit. And so we make these claims about the progression of disease. I don’t know that we have any really great studies, at least not here in the United States, regarding what happens with the progression typically.
Peter L. Salgo, MD: Well, instead of saying we understand how it progresses, at least we can ask how to assess how bad it is. What are the tools you’ve got at your disposal?
Joel Gelfand, MD, MSCE, FAAD: Well, I think it’s really a clinical assessment in terms of how bad the disease is. There are research assessments we use, but then there’s also clinical assessments we use and there are 2 perspectives. One is the objective doctor’s perspective—how extensive is the disease. Classically, we think that when psoriasis affects more than 10% of your body surface area, that’s considered to be severe disease, if you will. But special sites are important as well. There are some areas that we know cause a lot of burden for our patients. The scalp is very hard to treat with just traditional topical medications, for example. The nails are visible and often very disabling for patients, or the palms and soles can be very disabling. The genital area can be very disabling for patients. You could imagine a scenario where someone’s got a very localized psoriasis, but it could be severe because it really impacts a patient’s well-being, their quality of life, their social interactions, things of that nature.
Newsletter
Stay ahead of policy, cost, and value—subscribe to AJMC for expert insights at the intersection of clinical care and health economics.