Abstract Recap: Real-World Treatment Patterns Among Patients With Moderate to Severe Plaque Psoriasis by Metabolic Syndrome Status
Background
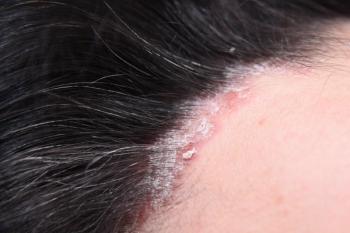
Psoriasis is a chronic, inflammatory disease that affects the skin.1 Compared with patients without psoriasis, those who have the condition are more likely to have metabolic syndrome,1 which encompasses a cluster of metabolic risk factors, such as insulin resistance and obesity, that increase a person’s risk of developing cardiovascular disease.2 An analysis of data from the National Health and Nutrition Examination Survey from 2003 to 2006 showed that about 40% of participants with psoriasis had metabolic syndrome.1
Patients with moderate to severe psoriasis may require biologic therapy or other treatment to address inflammation.3,4 However, few studies have examined the long-term real-world treatment patterns of patients prescribed these therapies, particularly among patients with metabolic syndrome.5
Methods
Investigators analyzed data from a large US claims database and classified eligible adult patients with psoriasis into 1 of 5 cohorts based on whether they received a prescription for adalimumab (ADA), apremilast (APR), etanercept (ETA), secukinumab (SEC), or ustekinumab (UST) as their initial index medication between January 1, 2015, and August 31, 2018. Patients were further stratified into subgroups based on whether any diagnosis of metabolic syndrome was recorded during the 12 months prior to the index period. To be included in the analysis, patients had to have continuous medical and pharmacy benefits during the 12 months before and 24 months after the index period and could not have used the index medication during the 12 months prior.5
Rates of adherence, discontinuation, nonpersistence, and switching were then compared among the cohorts. Adherence was determined based on proportion of days covered. Treatment gaps defined for each medication were as follows: 4 weeks for ETA and APR, 8 weeks for ADA, 10 weeks for SEC, and 18 weeks for UST.5
Results
A total of 7773 patients met the inclusion criteria. About half of patients in each cohort had metabolic syndrome: ADA, 50.6%; APR, 55.2%; ETA, 52.5%; SEC, 56.7%; and UST, 47.5%.5
During the 24 months after the index period, patients with metabolic syndrome had higher rates of discontinuation than those without metabolic syndrome across all cohorts except APR, as shown in
Conversely, patients with metabolic syndrome and those without showed similar rates of adherence, as shown in
Conclusions
Maintenance of long-term, self-administered therapy remains a challenge for patients with moderate to severe psoriasis, regardless of whether they also have metabolic syndrome. Adherence to medication was poor, and rates of nonpersistence and discontinuation were high among all treatment cohorts.5
References
1. Love TJ, Qureshi AA, Karlson EW, Gelfand JM, Choi HK. Prevalence of the metabolic syndrome in psoriasis: results from the National Health and Nutrition Examination Survey, 2003-2006. Arch Dermatol. 2011;147(4):419-424. doi: 10.1001/archdermatol.2010.370.
2. Grundy SM, Cleeman JI, Daniels SR, et al; American Heart Association; National Heart, Lung, and Blood Institute. Diagnosis and management of the metabolic syndrome: an American Heart Association/National Heart, Lung, and Blood Institute Scientific Statement. Circulation. 2005;112(17):2735-2752. doi: 10.1161/CIRCULATIONAHA.105.169404.
3. Menter A, Strober BE, Kaplan DH, et al. Joint AAD-NPF guidelines of care for the management and treatment of psoriasis with biologics. J Am Acad Dermatol. 2019;80(4):1029-1072. doi: 10.1016/j.jaad.2018.11.057.
4. Frequently asked questions about Otezla. Otezla website. otezla.com/plaque-psoriasis-treatment/faq. Accessed November 19, 2019.
5. Feldman S, Zhang J, Martinez D, et al. Real-world treatment patterns of biologics and apremilast among patients with moderate to severe plaque psoriasis by metabolic syndrome status [abstract L11]. J Manag Care Spec Pharm. 2019;25(suppl 10-a):S78. doi: 10.18553/jmcp.2019.25.10-a.s1.