Supplements and Featured Publications
- Contemporary Management of Moderate to Severe Plaque Psoriasis
- Volume 23
- Issue 21
Contemporary Management of Moderate to Severe Plaque Psoriasis
Am J Manag Care. 2017;23:S403-S416
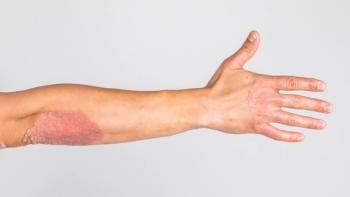
Psoriasis is a multisystem inflammatory disease that is often underdiagnosed, leaving many patients untreated. Plaque psoriasis, the most common form of the disease, affects approximately 80% to 90% of patients with psoriasis. Formulating a treatment plan can be complicated when various factors are considered. For example, type of therapy is dependent on the severity of the disease. Topical agents are preferred for mild disease, while phototherapy alone or in combination with systemic agents is recommended for the treatment of moderate to severe plaque psoriasis. Traditional systemic agents have the convenience of oral dosing; however, their toxicity profile can be a limiting factor. Newer biologic agents haven proven efficacious, if not superior to traditional oral agents, but their high cost can be a substantial disadvantage. Psoriasis has also been associated with increased risk of developing comorbidities, such as cardiovascular disease, obesity, and psoriatic arthritis, all of which increase the patient’s overall mortality and further worsen their overall physical well-being. Management of these comorbidities is often overlooked. Moreover, psoriasis may affect a patient’s psychological and social well-being. Patients with psoriasis are at a higher risk of developing clinical depression than patients without psoriasis. Inadequate management of comorbidities inevitably leads to poor outcomes, which increases the economic burden to the patient and society. Prevention and management of comorbidities, including cardiovascular and mental health, must be addressed as a part of a patient’s overall treatment plan. Specialist coordination may be beneficial for patients with psoriasis. Improved patient care may lead to better clinical and economical outcomes.Psoriasis is a multisystemic inflammatory disease that can substantially affect patients’ QoL (QoL). Psoriasis is characterized by skin papules, and plaques that are scaly, erythematous, painful, and pruritic.1 As a chronic condition, episodes of symptoms wax and wane over a patient’s lifetime and few patients experience spontaneous remission.1 Because this condition is frequently underdiagnosed, many patients with psoriasis remain untreated.2
In an analysis of National Health and Nutrition Examination Survey (NHANES) data collected from 2009 through 2010, the prevalence of psoriasis was 3.2% in Americans aged 20 to 59 years.3 Based on these data, it was estimated that in 2013 approximately 7.4 million adults older than 20 years were affected by psoriasis in the United States.3 However, this may be an underestimate of the true prevalence, as it did not account for those undiagnosed or patients with psoriasis who were younger than 20 years.3 Psoriasis is more common among adults than children, with 2 typical peaks of onset; the first peak at ages 20 to 30 years, and the second peak between ages 50 and 60 years.4 Psoriasis may be more common in non-Hispanic whites than in other ethnic groups.3 However, psoriasis is equally common in women and men.3
Plaque psoriasis, the most common form of psoriasis, affects approximately 80% to 90% of patients with psoriasis and is characterized by well-defined, erythematous plaques. Other forms of the disease include inverse, erythodermic, pustular and guttate psoriasis.1 Approximately 80% of patients with psoriasis have mild to moderate disease and the remainder have moderate to severe disease.2
Plaque Psoriasis Severity Rating Scales
Plaque psoriasis is diagnosed based on certain key physical manifestations. The well-defined erythematous plaques with white-silvery scales vary in size from 1 to a few centimeters. The irregular shaped plaques are most often located on the scalp, trunk, buttocks, limbs, and extensor surfaces. The severity of psoriasis is predominantly determined by the total body surface area (BSA) affected and the location, thickness, redness, and scaliness of the plaques; however, the impact of the disease on QoL is also an important consideration in clinical practice.2
Clinicians largely use BSA to evaluate psoriasis severity, as this value can be easily estimated in an office setting.5 The National Psoriasis Foundation (NPF) defines mild psoriasis as plaque affecting less than 3% of the BSA; moderate psoriasis as plaque affecting 3% to 10% BSA, and severe psoriasis as plaque affecting more than 10% BSA.6,7 Patients with mild disease may have only a few plaques covering less than 3% of BSA.6 Moderate to severe psoriasis is defined as psoriasis that affects 3% or more BSA or psoriasis present in vulnerable locations such as the hands, feet, face, and genital regions.1,6 The disease may also be considered more severe if it substantially impacts the patient’s psychological or physical well-being.2
Burden of Comorbid Conditions in Patients With Psoriasis
Psoriasis is associated with an increased risk of several medical comorbidities. The etiology behind this has not been fully elucidated, but presumably results from overlapping pathophysiology.8 It is known that the chronic inflammatory state characteristic of psoriasis affects other body systems. For example, chronic inflammation may predispose patients with psoriasis to obesity and atherosclerosis; or worsen these conditions if they are already present.8 Oxidative stress, common environmental factors, specific genes, psychosocial stressors, behavioral changes, and potential adverse therapy effects may also play an etiological role in these comorbidities.2,8,9
Cardiovascular Disease
Patients with psoriasis have greater risk of cardiovascular (CV) events, and greater severity of the disease is associated with higher CV event rates. An increased risk of CV events in patients with psoriasis may be associated with the underlying the abnormal physiology of psoriasis. Alternatively, the relationship may be due to poor lifestyle choices, driven by the psychological impact of psoriasis, that contribute to obesity and CV decline.10
A cross-sectional study of more than 130,000 patients with psoriasis in the United Kingdom found an increased prevalence of diabetes (7.1% vs 3.3%), hypertension (20% vs 11.8%), elevated lipid levels (6% vs 3.3%), and smoking (30.1% vs 21.3%) compared with patients without psoriasis, respectively.11
The relationship between CV disease (CVD) and psoriasis was further demonstrated in a retrospective analysis of claims data from 2 large US healthcare databases. Patients with psoriasis demonstrated a 1.2-fold greater risk of atherosclerosis, congestive heart failure, type 2 diabetes (T2D), and peripheral vascular disease than patients without psoriasis. The highest rates of CVD or risk were demonstrated in patients with more severe psoriasis compared with mild disease.10
Patients with psoriasis also have an increased risk of overall mortality, largely due to CVD.2 Patients with severe psoriasis are 39% more likely to experience fatal CV events compared with patients without psoriasis (rate ratio [RR], 1.39; 95% CI, 1.11-1.74). Fatal cardiovascular events occur at an incidence rate of 2.1 to 16.2 per 1000 person-years in this population (
A recent prospective study of patients with psoriasis patients in the United Kingdom demonstrated an increased risk of early death, which was associated with comorbid CV conditions.13 Differences in mortality rates were investigated in adults with psoriasis (N = 8760) and without psoriasis (N = 87,600) after adjusting for confounders such as age, sex, and comorbidity scores. The investigators identified higher rates of multiple chronic diseases in patients with plaque psoriasis, including chronic kidney disease, diabetes, chronic obstructive pulmonary disease, and past myocardial infarction. Mortality rates were comparable between patients with and without psoriasis: 3.35 deaths per 1000 person-years compared with 2.12 deaths, respectively. However, in a stratified analysis of patients with psoriasis by BSA affected, patients with more than 10% of BSA affected had a significantly increased risk of mortality versus patients without psoriasis (HR, 2.12, 95% CI, 1.46-3.07). This increased mortality risk remained even after adjustment for comorbidities (HR, 1.79; 95% CI, 1.23-2.59).13
Metabolic Syndrome
Patients with metabolic syndrome are predisposed to coronary heart disease. Metabolic syndrome is defined as the presence of at least 3 of 5 specified metabolic risk factors in a single individual. These factors include elevated fasting glucose, elevated blood pressure, elevated triglycerides, and increased waist circumference.14 Patients with psoriasis were found to be at a greater risk of meeting the metabolic syndrome criteria (odds ratio [OR], 1.7-5.3).14 The underlying chronic inflammation of psoriasis may be a contributing factor in the pathophysiology of insulin resistance, visceral adiposity, hypertension, and dyslipidemia.9 Metabolic syndrome is also more likely in patients with severe psoriasis compared with those with mild disease.8
Obesity deserves special mention as a comorbidity in psoriasis. It contributes to a number of different health conditions, including CVD, T2D, obstructive sleep apnea, and osteoarthritis.15 Obesity has profound social and psychological impacts on patients. Obese patients report lower self-esteem due to social stigmatization and concerns about their appearance, and they experience bias in areas such as education and employment.16 A meta-analysis of 16 cross-sectional and case controlled studies showed that patients with psoriasis have greater than 50% odds of being obese compared with the general population. Moreover, the OR for obesity was significantly higher for patients with moderate to severe psoriasis compared with patients with mild disease. Additionally, patients with pre-existing psoriasis have a greater likelihood of becoming obese than do patients without psoriasis.15
A variety of mechanisms have been proposed for the association of obesity and psoriasis. These include underlying genetic and inflammatory mediators or adverse effects from certain medications.15 Psoriasis might also increase the risk of obesity via increased depression, alcohol use, and social isolation, as well as unhealthy eating habits and decreased physical activity.14 The association also proceeds in the other direction, as obesity may increase the risk of developing psoriasis.14 Partly as a result of this association, individuals with psoriasis are also at greater risk of T2D.17
Psoriatic Arthritis
Psoriatic arthritis (PsA) is another major comorbidity occurring in a subgroup of patients with psoriasis. The incidence of PsA is unclear, but a meta-analysis placed it at approximately 6.4 per 100,000. In patients with psoriasis, the prevalence estimates range from 6% to 41%.18 It most commonly presents as an asymmetrical oligo-arthritis causing pain and swelling in the affected joints.18 The condition can sometimes predate skin problems, but more commonly appears in patients already exhibiting psoriasis.18 Notably, those with PsA can also have significant extra-articular comorbidities affecting the tendons and ligaments, eyes, gastrointestinal tract, heart, arteries, and urogenital system.18
In addition to these major more common comorbidities, psoriasis also increases the risk of other medical conditions. The risk of Crohn’s disease in patients with psoriasis is estimated to be between 3.8 and 7.5 times greater compared with the general population and patients with psoriasis may have a higher risk of multiple sclerosis and lymphoma.2
Psychological Distress and Mental Health
Patients with psoriasis often feel stigmatized by their physical appearance, which may contribute to comorbid social isolation and stress-related disorders, such as depression and anxiety.19 Some evidence suggests that depression is more common in patients with psoriasis than in patients with other skin disorders, such as lichen planus or vitiligo.20 Prevalence estimates of depression in patients with psoriasis range from 6% to 62% depending on study-related factors (eg, design, population enrolled, definition criteria).19 A meta-analysis used pooled data from 98 studies to determine the prevalence and odds of depressive symptoms and clinical depression in patients with psoriasis. Of a large population of patients with psoriasis (N = 401,703), 28% showed symptoms of depression. Overall, patients with psoriasis were 1.5 times more likely to have clinical depression; approximately one-tenth were diagnosed according to the Diagnostic and Statistical Manual of Mental Disorders (DSM) IV criteria.19
Depression and psoriasis appear to have a complex pathophysiological relationship. In the United States, women with depression are more likely to experience new-onset psoriasis than men.20 In addition, a clear relationship has been elucidated between inflammation and depression; however, the extent of the pathological influence of depression or inflammation to each condition is unclear.21 Excessive alcohol use, which can exacerbate mental health morbidities, is more prevalent in patients with psoriasis compared with those without psoriasis.22
In a meta-analysis evaluating the relationship between psoriasis and suicide, risk of suicidal ideation was increased 2-fold in patients with psoriasis compared with patients without psoriasis (OR, 2.05; 95% CI, 1.54-2.74). Patients with psoriasis were also 32% more likely to attempt suicide (OR, 1.32; 95% CI, 1.14-1.54) and 20% more likely to complete suicide (OR, 1.20; 95% CI, 1.04-1.39).23 The severity of psoriasis was directly correlated with suicidal ideation and suicide attempts, where patients with more severe psoriasis were more likely to consider suicide and attempt suicide compared with those with more mild disease.23
The many medical comorbidities associated with psoriasis can decrease QoL. Worries about medical conditions and their consequences can put additional strains on mental health and further contribute to depression and anxiety.24 Conversely, poor mental health can exacerbate the health outcomes of these comorbidities. For example, patients with untreated depression may be less likely to take proper health preventative measures, and may demonstrate decreased ability to manage their needed medications.25 An analysis of NHANES data collected from over 30,000 patients demonstrated major depression in addition to a major medical condition is associated with greater healthcare utilization, more days spent in bed, greater functional disability, and higher productivity losses compared with patients without major depression.26
The comorbidity of PsA represents an additional psychological strain for patients with psoriasis. Patients with PsA have worse functional status, greater disability, and poorer QoL than patients with psoriasis who do not have PsA.27 Results of a large prospective cohort study also demonstrated an increased risk of incidence depression in women with psoriasis after adjusting for potential confounders, and an even greater risk for women with PsA. Multivariate-adjusted RRs of clinical depression were 1.29 (95% CI, 1.10-1.52) for women with psoriasis and 1.52 (95% CI, 1.06-2.19) for women with psoriasis and concomitant PsA compared with women without psoriasis.28
The impact of PsA on depression and suicidal ideation was investigated in patients with psoriasis. More than 36,000 patients with psoriasis, over 5000 patients with PsA and nearly 1900 patients with ankylosing spondylitis were enrolled. After adjusting for measurable confounders, all 3 study populations demonstrated an increased risk of depression. The IRR for psoriasis, PsA, and ankylosing spondylitis were 1.14 (95% CI, 1.11-1.17), 1.22 (95% CI, 1.16-1.29), and 1.34 (95% CI, 1.23-1.47), respectively.29 When researchers examined an endpoint that encompassed both suicidal ideation and suicide attempts, this measure was significantly higher in patients with PsA compared with the general population. In this study, this risk was not elevated in patients who had psoriasis alone or in patients with ankylosing spondylitis.29 In 2017, the results of large prospective study of over 73,000 patients demonstrated that major depressive disorder increases the risk of PsA development as much as 37% in patients with psoriasis. In this way, managing depression in patients with psoriasis may be an important consideration for clinicians.30
Economic Burden of Psoriasis
Management of psoriasis can place a large economic burden on patients, especially those with more severe disease.31 Costs include direct disease expenses, costs from disease morbidities, and indirect costs such as from lack of productivity at work. Additional indirect costs can stem from restriction of activities and poor self-esteem due to the condition.32 In an analysis of data from 22 studies investigating costs associated with psoriasis in the United States, investigators estimated the annual overall economic burden of psoriasis ranged from $112 billion to $135 billion in 2013.32 The annual direct costs of psoriasis accounted for $52 billion to $64 billion of this total annual burden.32
In an analysis of a large US healthcare database, healthcare claims from 18,653 patients with psoriasis were used to categorize patients by all-cause total costs from 2011 to 2013, including healthcare resource utilization, treatment, and comorbidities costs. Patients in the highest-cost group accounted for 2.8% (n = 514) of all patients in the study, while patients in the lowest cost group (bottom 90% of expenditures in all 3 years), accounted for 79.8% (n = 14,891) of the study population.33 From 2011 to 2013, expenditures in the highest-cost group accounted for 13.3% to 13.7% of total annual costs, and 3.3% to 4.6% of psoriasis-related costs. All-cause costs this group were also 7.8-fold higher than in the lowest cost group with $68,913 and $8815, respectively. The lowest cost group accounted for approximately half of all-cause costs (50.7%-51.8%) and the majority of psoriasis-related costs (69.2%- 74.6%).33 Psoriasis-related medical and pharmacy costs were also higher in the highest-cost group ($8716) compared with the lowest-cost group ($4541).33
The management of comorbidities was the greatest expenditure contributing to the total economic burden of psoriasis.33 The highest-cost group presented with more comorbidities and there were significantly more patients with moderate or severe psoriasis in this group (40.7% vs 32.3%; P <.001). Patients in the group with the highest costs also had significantly more hospitalizations (36.8% vs 2.6%; P <.001) and psoriasis-related hospitalizations (11.1% vs 0.7%; P <.001) compared with the lowest-cost group.33
The annual costs of medical comorbidities in patients with psoriasis have been estimated at $36 billion in the United States.32 In patients with moderate to severe disease, a comorbid psychiatric disorder has the potential to add several thousands of dollars annually per patient.32 PsA, diabetes, hypertension, and obesity are just a few of the comorbid conditions that drive costs in the management of patients with psoriasis.32 Patients with comorbidities have higher direct and indirect costs, and require the use of more healthcare resources (
Without the inclusion of costs from medical comorbidities, the annual indirect costs from psoriasis have been estimated to range from $24 billion to $35 billion annually, including losses from work absenteeism and reduced work productivity (
Patients with psoriasis have reported discrimination at work and difficulty in certain career paths related to their condition.36 The NPF investigated the impact of psoriasis on work status by analyzing survey data from more than 5600 patients with psoriasis (
Assessing Treatment Response
There are no measurable biomarkers that correlate with psoriasis severity. Clinicians often rely on clinical scoring systems to assess treatment response.38 The lack of clearly defined consensus treatment targets in psoriasis complicates analysis of best disease management.6
Psoriasis assessment tools, such as the Psoriasis Area and Severity Index (PASI), are often used in clinical trials. PASI scoring provides a uniform, objective measure of severity for comparison; thereby, reducing investigator bias.39 In clinical trials, the PASI is the traditional standard for assessing degree of psoriatic skin involvement.40 PASI provides a composite measure of both the signs and extent of psoriasis, entered into a formula that yields a score from 0 to 72.38,40 When comparing the efficacy of treatment options, researchers often rely on the PASI score as a measure of efficacy. A PASI success rate is reported as the percentage of patients that achieve a specific level of clearance of disease.41 A PASI 75 response represents a 75% reduction in the PASI score from baseline, or 75% disease clearance from the start to end of a clinical trial. PASI 90 represents a 90% reduction in the PASI score from baseline. Only the PASI 100 response measure represents total disease clearance.40
Although the PASI is a commonly used disease assessment tool, other measures are also used to assess psoriasis severity, such as BSA and the Physician Global Assessment (PGA), which provides an ordinal scale to assess psoriasis severity.38 In addition, the combined score of these 2 measures, known as s-MAPA, can also be used to assess disease severity.42 Other scoring metrics were developed with an intent to simplify PASI scoring. The Psoriasis Assessment Severity Score (PASS) and the simplified PASI (SPASI) were derived from PASI.38 In an effort to develop a more accurate measure of severity, the Psoriasis Log-Based Area and Severity Index (PLASI) and the Psoriasis Exact Area Severity Index (PEASI) were designed to include other important factors that the PASI score fails to consider.38
Clinical Practice Guidelines in the Treatment of Plaque Psoriasis
Guidelines for the management of plaque psoriasis developed by the American Academy of Dermatology indicate that treatment for psoriasis is guided by measures of disease severity (
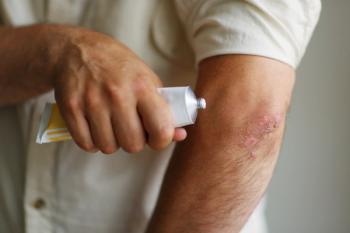
Additional therapies for the treatment of plaque psoriasis may be needed for patients for whom treatment fails or who have more severe and extensive disease. As an alternative treatment option for these patients, phototherapy may provide effective and economical management without the potential toxicities of traditional and biologic therapies. Phototherapy can be administered in combination with topical agents, traditional systemic agents, or biologics for patients with moderate or severe disease.2 However, phototherapy may be limited by a lack of accessibility and inconvenient time commitment.2
Clinicians may escalate treatment with the use of traditional oral systemic agents for patients who do not achieve adequate response with phototherapy or topical treatment. Typically, an oral systemic agent is used for patients with initially extensive disease or severe psoriasis (BSA >10%). However, traditional oral systemic agents may also be appropriate for patients with limited disease with greater psoriasis symptoms which affect their QoL.44 Methotrexate, cyclosporine and the retinoid, acitretin, have been routinely used in clinical practice and have established long-term efficacy and organ toxicity profiles.2 Potential organ toxicities of oral systemic agents include liver, bone marrow, and kidney complications.44 In this way, patients must be carefully selected for treatment with traditional oral systemic agents and routinely monitored for adverse outcomes. Traditional oral systemic agents have a greater risk of organ toxicity compared with newer biologic agents.44
Biologic agents target specific molecules involved in the development of psoriatic plaques.1,2 In 2003, the FDA approved the first biologic agents that revolutionized psoriasis treatment.45 The introduction of newer agents provide additional options for patients with plaque psoriasis who require systemic treatment, as these newer agents may provide more effective and less toxic treatment alternatives compared with oral agents.2,44
Biologic agents vary in their mechanisms of action, mode of administration (subcutaneous or intravenous), immunogenicity, cost, availability within health plans, and indications for first or second-line therapy in the treatment of plaque psoriasis.46 Apremilast is an oral, nonbiologic agent indicated for the treatment of patients with moderate to severe plaque psoriasis.47 Its oral formulation provides an alternative to patients who may be unhappy with other treatments due to ineffectiveness, intolerability, or injection problems.48
Considerations in Treatment Selection and Efficacy Outcomes
As annual costs for biologics have been estimated to range from $13,000 to $30,000 per patient in the United States, considerations of treatment choice are important.41 Physicians and managed care professionals may also have different views about the selection of oral agents compared with biologic treatment due to the high costs and administration requirements of biologics.31 Payers may promote a step-wise treatment approach for moderate to severe psoriasis, incentivizing traditional systemic drugs as first-line treatments for patients who require escalated therapy. In contrast, physicians may prefer to initiate treatment with a more expensive biologic drug in patients with extensive disease.1,49
Costs from inadequately controlled disease, indirect costs, and expenses from worsening medical comorbidities may be considered when evaluating the cost-effectiveness of agents for the treatment of plaque psoriasis. Limitations of current investigations of cost analysis between biologics and oral agents include that studies do not account for costs of inadequately treated medical morbidities or adverse events (AEs) associated with the treatment selection and do not incorporate the effects of rapid treatment and sustained clearance. Moreover, cost comparisons have often used PASI 75 as a standard treatment goal despite this outcome reflecting an incomplete or nonresolution of psoriasis.31
The relationship between cost and physical and psychological functioning, as well as QoL was evaluating the relationship between measures of disease severity using the Dermatologic Life Quality Index (DLQI) and PASI and costs from a societal perspective in patients with plaque psoriasis not receiving biologic treatment. A stronger correlation was demonstrated between DLQI and cost compared with PASI and cost.50 Of patients not receiving biologics, high levels of impairments on the DLQI had greater overall costs, including indirect costs such as productivity losses. Patients receiving systemic therapy also had higher costs.50 Patients with a higher DLQI had higher costs associated with their plaque psoriasis compared with patients with less DLQI. The main cause of the cost discrepancy was lost production, followed by topical medication cost.50 The investigators concluded that biologics should be considered in patients with high DLQI scores.50
When comparing clinical trials, an important consideration arises from the changes in scoring metrics used to measure outcomes. In earlier trials, PASI 75 was the standard therapeutic goal and benchmark in many studies investigating. 45 However, with the advent of newer treatments PASI 90 and PASI 100 is becoming the emerging standard for evaluating therapeutic goals.40,45 Growing evidence supports the idea that PASI 90 and PASI 100 should be the new gold standard of efficacy assessment. Greater control and clearance of plaque not only manages the disease itself, but may also improve patients’ physical and psychological functioning and QoL, as assessed by the DLQI. 40
PASI values may be less beneficial in an immediate clinical setting. To help clinicians develop consistent targets in the management of plaque psoriasis, the NPF medical board conducted a consensus-building study.6 Using the Delphi technique, 25 experts from the NPF indicated that BSA was their preferred instrument to assess plaque psoriasis severity in clinical practice.6 The expert panel considered an acceptable response to initial therapy to be either an affected BSA of 3% of less, or a 75% or greater improvement from baseline to 3 months after treatment began.6 After this 3-month period, the experts recommend a treatment target BSA of 1% or less, with assessments at 6-month intervals throughout maintenance therapy.6
Following these recommendations, Wu and colleagues proposed a new nomenclature for BSA, such that a 75% improvement in BSA would be recognized as BSA 75, a 90% improvement would be noted as BSA 90, and a 100% improvement would become BSA 100. Such a classification schema would be analogous to improvements in the PASI 75, PASI 90, and PASI 100, respectively.5 These guidelines might serve as practical and straightforward tools to help clinicians monitor treatment response.5
Primary Endpoints in Clinical Trials
Patients with psoriasis who have an incomplete response to treatment may demonstrate substantial symptom burdens and effects on health-related QoL.51 In a secondary analysis of the phase 3 AMAGINE -1, AMAGINE -2, AMAGINE -3 trials, investigators pooled data from patients in the brodalumab arms who achieved at least PASI 75 during the trials to evaluate if achievement of complete skin clearance (PASI 100) significantly improved patient-reported QoL (DLQI) scores compared with patients who were almost cleared of the disease (PASI 75 or PASI 90). A greater proportion of patients who achieved PASI 100 demonstrated an absence of interference of psoriasis on daily life (DLQI score of 0 or 1) compared with patients who were almost clear of disease; 62.7% of patients with skin clearance between PASI 90 and PASI 100 had DLQI scores of 0 or 1, compared with 80.2% of patients who achieved PASI 100 with brodalumab treatment. Additionally, a greater proportion of patients with PASI 100 had symptom-free days during the 12 weeks of follow up compared with patients who had skin clearance between PASI 75 and PASI 100 (10.5% vs 42.3%).51
The evolution of PASI endpoints deserves special consideration, as managed care providers may set standardized treatment goals at PASI 75. Earlier investigations of the safety and efficacy of agents used to treat psoriasis utilized PASI 75 as a primary end point, although PASI 90 was a key trial outcome.52-54 PASI 75 was a reasonable target for drugs such as tumor necrosis factor (TNF) inhibitors, reflecting their overall efficacy.45 Some newer trials of potentially more efficacious drugs are still continuing to use PASI 75 as a primary endpoint, although PASI 90 and PASI 100 are often reported as secondary measures.48,55-57 PASI 75 is still the most commonly used measure of treatment response.58
Recent trials investigating biologics for the treatment of moderate to severe plaque psoriasis have set primary end points as the achievement of PASI 90.59-61 PASI 90 and complete skin remission measured as PASI 100 in response to treatment may be a reasonable goal, given the increased rate of response seen with newer biologic agents.58 In phase 3 trials of the interleukin (IL)-17 inhibitory agents secukinumab, ixekizumab, and brodalumab, PASI 90 was achieved at Week 12 in 59%, 71% and 70% of patients, respectively.57,62,63 As a measure of reference, European and Canadian guidelines have adopted PASI 100 as the standard treatment goal for psoriasis.64 According to the NPF, treatment targets for psoriasis an acceptable response at 3 months after treatment initiation is achieving BSA 3% or less, or BSA improvement of at least 75% from baseline. Clinicians and patients should strive to achieve a target response of BSA 1% or less at 3 months after treatment initiation and at every 6-month evaluation with maintenance treatment.6
The etiological role of chronic inflammation is another important consideration in targeting treatment goals. The chronic inflammation found in psoriasis is also thought to play a causal role in its comorbidities, including obesity, metabolic syndrome, atherosclerosis, and depression.8,21 Treatments for psoriasis help address aspects of this inflammation, and achievement of higher PASI 75, PASI 90, and PASI 100 may reflect better controlled systemic inflammation overall. Targeting a higher therapeutic PASI goal may positively impact these comorbidities through decreasing overall systemic inflammation. However, there is insufficient consolidated data to state this definitively at this time.8
Current Agents in the Treatment of Moderate to Severe Plaque Psoriasis
Recent systemic treatment options for the management of moderate to severe plaque psoriasis fall into 2 classes of agents: biologic and nonbiologic. Biologic agents compose the majority of the most efficacious drugs to treat psoriasis (
TNF Inhibitors
Etanercept
TNF alpha (TNFα) is an inflammatory cytokine believed to be a key mediator of inflammation in the pathogenesis of psoriasis.53,54 Etanercept competitively binds to cell-surface receptors and inhibits endogenous TNF-mediated receptor activation. Etanercept is indicated for the treatment of moderate to severe plaque psoriasis in patients who are candidates for systemic or phototherapy.65 In an early phase 3 trial, patients with clinically stable plaque psoriasis were randomized to treatment with high-dose (50 mg) etanercept (N = 164) or placebo (N = 166). The primary efficacy end point was the proportion of patients achieving PASI 75 at Week 12. In the etanercept treatment group, 49% of patients achieved PASI 75 and 22% achieved PASI 90 at Week 12 compared with 4% and 1% of placebo treated patients, respectively. Patients treated with etanercept continued response at the 24-week assessment; 59% achieved PASI 75 and 30% achieved PASI 90.53
Infliximab
Infliximab is indicated for the treatment of adult patients with chronic severe plaque psoriasis who are candidates for systemic therapy when other systemic treatment options are not deemed medically appropriate.66 Infliximab is a monoclonal antibody that binds and neutralizes the biological activity of TNFα.54 The phase 3 EXPRESS trial evaluated the safety and efficacy of infliximab in patients with moderate to severe plaque psoriasis. Of the 301 patients randomized to treatment with infliximab, 80% achieved PASI 75 and 57% achieved PASI 90 at Week 10 compared with 3% and 1% of placebo treated patients, respectively. Although patients maintained response to infliximab at Week 24, after 50 weeks of treatment, the proportion of patients that achieved PASI 75 and PASI 90 decreased to 61% and 45%, respectively.54
Adalimumab
Adalimumab is an anti-TNFα monoclonal antibody indicated for the treatment of patients with moderate to severe plaque psoriasis.1 The long-term efficacy and safety of adalimumab was investigated in the REVEAL phase 3 trial. In the REVEAL trial, 71% of the patients receiving adalimumab achieved PASI 75, 45% achieved PASI 90 and 20% achieved PASI 100 at Week 16.68 Week 24 data shows there was a slight increase in patients that achieved PASI 90 and PASI 100 (49% and 22%, respectively).68 The ESPRIT Registry is an ongoing, 10-year postmarketing surveillance registry that is tracking the long-term safety and efficacy of adalimumab in the real world environment outside of a clinical trial. The results from the 7-year interim analysis shows the as-observed effectiveness has either increased or remained stable through the 7 years of the registry thus far.75
Some evidence suggests TNF inhibitors may have a positive effect on depression that may be attributed to mediation of anti-inflammatory effects. The results of a phase 3 trial of etanercept showed that patients treated with the drug had less fatigue and depression as assessed by the Beck Depression Inventory (BDI), the Hamilton Rating Scale for Depression (HRSD), and the Functional Assessment of Chronic Illness Therapy Fatigue scale (FACIT-Fatigue).76 Similarly, a trial of adalimumab found that the drug seemed to reduce symptoms of depression in patients with moderate to severe psoriasis.77
Biosimilars may lower the cost of treating moderate to severe plaque psoriasis. Biosimilars of adalimumab and etanercept were approved for chronic moderate to severe plaque psoriasis and biosimilars of infliximab were approved for chronic severe plaque psoriasis.78-82
IL-12/23 Inhibitor
Ustekinumab
IL-12 and IL-23 have been shown to play an important role in psoriasis pathogenesis, and several available products modulate the levels of these cytokines.52 Ustekinumab is an monoclonal antibody which binds to a subunit shared by IL-12 and IL-23.52 Theresults from the phase 3 PHOENIX-1 and PHOENIX-2 trials demonstrated that at Week 28, 79% of patients with moderate to severe plaque psoriasis achieved PASI 75 in both trials; 54% and 55% achieved PASI 90 and 29% and 30% achieved PASI 100 at the highest dose (90 mg) in PHOENIX-1 and PHOENIX-2, respectively. Patients that discontinued ustekinumab treatment due to unsatisfactory therapeutic effect were deemed treatment failures.52,70 Analysis of the phase 3 PHOENIX-2 trial also showed that ustekinumab treatment improved symptoms of anxiety and depression as measured by the Hospital Anxiety and Depression Score (HADS) and the DLQI.83 Five patients experienced AEs of depression which later normalized.83
IL-17 Inhibitors
Recently developed biologics target IL-17, a pro-inflammatory cytokine whose production is closely dependent on the production of IL-23.45,58 Secukinumab and ixekizumab are agents that target the IL-17A ligand, while a similar drug, brodalumab, targets the IL-17RA receptor subunit which is thought to be shared by several other ligands in the class.58
Secukinumab
The phase 3 ERASURE trial of secukinumab found that at Week 12, 82% of patients receiving secukinumab 300 mg achieved PASI 75, 59% achieved PASI 90, and 29% achieved PASI 100.57 The phase 3 FIXTURE trial of secukinumab found similar results, with patients achieving PASI 75, PASI 90, and PASI 100 were 77%, 54%, and 24%, respectively.57 Missing data were imputed conservatively as nonresponses regardless of the reason for missing data.57
Ixekizumab
The safety and efficacy of ixekizumab in patients with moderate to severe psoriasis were evaluated in the UNCOVER-1, UNCOVER-2, and UNCOVER-3 phase 3 trials. The UNCOVER-1 trial compared ixekizumab with placebo. In the group receiving ixekizumab every 2 weeks for the first 12 weeks followed by every 4 weeks, 89% of the achieved PASI 75; 71% achieved PASI 90; and 35% achieved PASI 100.55 At Week 60, the proportion of these patients that achieved PASI 75, PASI 90, and PASI 100 were 80%, 73%, and 55%, respectively.55 The UNCOVER-2 and UNCOVER-3 trials compared ixekizumab with placebo and an active comparator, etanercept. The 2 respective trials showed that 90% and 87% of patients achieved PASI 75, 71% and 68% achieved PASI 90 and 41% and 38% achieved PASI 100 at Week 12 in the group receiving ixekizumab every 2 weeks compared with the relative rates of 42% and 53%, 19% and 26%, and 5% and 7% in the etanercept group.55,62
Brodalumab
Brodalumab is a human IL-17 receptor antagonist indicated for the treatment of adult patients who have failed to respond or lost response to other systemic therapies.69 The safety and efficacy of brodalumab were studied in the phase 3 trials, AMAGINE-1, AMAGINE-2, and AMAGINE-3. The AMAGINE-1 trial compared brodalumab with placebo and showed that 83% of the patients receiving brodalumab achieved PASI 75, 70% achieved PASI 90, and 42% achieved PASI 100 at Week 12.73 Brodalumab was compared with placebo and an active comparator, ustekinumab, in the AMAGINE-2 and AMAGINE-3 trials. In the 2 respective trials, the proportion of patients that achieved PASI 75 at Week 12 were 86% and 85% in the brodalumab groups versus 70% and 69% in ustekinumab groups.64 The proportion of patients that achieved PASI 90 at week 12 were 70% and 69% in the brodalumab groups versus 47% and 48% in ustekinumab groups.64 Patients that achieved PASI 100 at Week 12 were 44% and 37% in the brodalumab groups versus 22% and 19% in the ustekinumab groups.64 At Week 52, the proportion of patients in the brodalumab groups that achieved PASI 75, PASI 90, and PASI 100 in the AMAGINE-2 and AMAGINE-3 trials were 80% in both trials, 75% and 73%, and 56% and 53%, respectively; compared with the respective rates in the ustekinumab groups of 62% and 63%, 48% and 50%, and 29% and 30%.64
Concerns for psychiatric adverse effects have also been raised for brodalumab. Four completed suicides (including an indeterminate one) were reported during the brodalumab psoriasis trials, which was higher than expected.84 However, it is uncertain whether there is a true association between brodalumab and increased rate of suicide due to the presence of confounding variables during the trials. The brodalumab trials’ exclusion criteria did not exclude patients with mental health comorbidities as rigorously as most clinical trials evaluating systemic drugs in patients with moderate to severe psoriasis. The exclusion criteria were designed to mimic the general psoriasis population more accurately.85 Baseline psychiatric disorders, including depression and anxiety, were present in 18% of the patients.85 Furthermore, no increase in suicidal behavior events was seen during the trial in the brodalumab treatment group.84,85 The investigators also found that a greater proportion of patients in the brodalumab group had improved anxiety or depression symptoms, based on the HADS criteria, compared with patients receiving placebo.85
Some newer clinical trials have excluded patients with severe depression, any history of depression or suicidal ideation, or other psychiatric disorders, partly because of the aforementioned concerns.86,87 Many trials have used strict exclusion criteria for mental health comorbidities, including studies of adalimumab, apremilast, certolizumab, secukinumab, and ustekinumab.88 Therefore, the studied populations may not be representative of all patients with plaque psoriasis, and may underestimate psychiatric risks associated with the general use of these drugs.
Selective IL-23 Inhibitors
Selective IL-23 inhibitors are an emerging class of biologic agents for the treatment of moderate to severe plaque psoriasis.
Guselkumab
Guselkumab was recently approved for the treatment of patients with plaque psoriasis following the results of the phase 3 studies VOYAGE 1 and VOYAGE 2.60 Guselkumab is a monoclonal antibody that blocks the downstream signaling of IL-23. In the VOYAGE 1 and 2 trials, the proportion of patients who achieved PASI 75 at Week 16 were 86% and 91%; PASI 90 was achieved by 70% and 73%; PASI 100 was achieved by 34% and 37%. In contrast, the respective rates in the active comparator (adalimumab) group at Week 16 were 69% and 73%, 47% and 50%, and 17% and 21%, respectively. VOYAGE 1 reported that at Week 48, the proportion of patients that achieved PASI 75 decreased to 88%, but increased for PASI 90 (76%) and PASI 100 (47%). The rates in the adalimumab group decreased for both PASI 75 (63%) and PASI 90 (48%), but increased for PASI 100 (23%).59,60
Tildrakizumab
Tildrakizumab and risankizumab are monoclonal antibody IL-23 inhibitors currently being evaluated in phase 3 trials for patients with moderate to severe plaque psoriasis. The FDA has accepted the biologics license application for tildrakizumab, which was filed based on results from the phase 3 reSURFACE 1 and reSURFACE 2 trials. Respective PASI 75 responders in the reSURFACE 1 and reSURFACE 2 trials were 62% and 66%, PASI 90 35% and 37%, and PASI 100 12% and 14% at Week 12 in patients receiving tildrakizumab. In comparison, patients receiving active comparator, etanercept, in the reSURFACE 2 trial were 48%, 21%, and 5%. Week 28 results from reSURFACE 1and reSURFACE that the proportion of patients receiving tildrakizumab increased for PASI 75, PASI 90, and PASI 100 to 79% and 73%, 57% in both trials, and 31% and 26%, respectively. Similarly, rates increased for PASI 75, PASI 90, and PASI 100 in the etanercept group with rates of 54%, 29%, and 11%, respectively.56
Risankizumab
Risankizumab is another anti—IL-23 monoclonal antibody. Currently, the safety and efficacy results from phase 3 trials, UltIMMa-1 and UltIMMa-2, have not been published to date.89,90 Results of the phase 2 study of risankizumab showed the proportion of patients in the risankizumab high-dose group at Week 12 that achieved PASI 75, PASI 90, and PASI 100 was 88%, 81%, and 48%, compared with 40%, 72%, and 18% response in the ustekinumab group, respectively.61
Nonbiologic Agents
Apremilast is a novel oral, nonbiologic agent that regulates inflammatory mediators through inhibition of phosphodiesterase-4.48 In the phase 3 ESTEEM-1 trial, 33% of patients with chronic plaque psoriasis who received apremilast achieved PASI 75 at Week 16 and 9.8% achieved PASI 90.48 Sixty-one percent of the patients who remained on apremilast through Week 52 achieved PASI 75 response at Week 52.48 Its toxicity profile is milder than traditional oral systemic agents; however, severe diarrhea, nausea, and vomiting can occur in the first few weeks of initiation. Apremilast also has been associated with an increased risk of depression.47 Physicians should carefully evaluate patients for depression prior to starting therapy, and closely monitor for its signs and symptoms while therapy is ongoing.47
Unmet Needs in the Burden of Psychiatric Morbidities
The common psychiatric comorbidities of psoriasis substantially impair QoL. It is important for clinicians to understand the true burden of these psychiatric issues, especially in patients with moderate to severe plaque psoriasis. Patients with psoriasis may perceive their mental and physical burdens to be greater than those of patients with cancer, arthritis, hypertension, heart disease, and diabetes.2 Patients believe that other people do not understand how much the disease negatively affects their lives.24
Although the frequency of psychiatric problems lessens with decreasing clinical symptoms, even patients with mild psoriasis can continue to experience substantial distress.91
Psoriasis profoundly affects QoL, even in patients who do not meet the full criteria for psychiatric illness. In a survey of over 5600 patients with psoriasis and PsA conducted by the NPF, psoriasis negatively affected the well-being of 88% of the population.37 Most patients experienced anger, helpless, embarrassment, and self-consciousness as part of their disorder. 37 Other studies’ results have demonstrated that, regardless of psoriasis severity, nearly 60% of patients believe psoriasis had a major impact on their QoL.92 Patients often report poor self-esteem and body image, as well as feeling of stigma from others.24 Uncontrolled disease impacts patients’ daily activities, work capabilities, social life, and sexual functioning.24
Psoriasis also deserves consideration as a dermatologic psychophysiological disorder. Such disorders are defined by the fact they can fluctuate in severity and may worsen in response to stress, anxiety, or depression.93 Psoriasis may be exacerbated as patients experience anxiety, embarrassment, or sadness about their disease. This promotes a vicious cycle, as emotional distress can worsen the physiological skin symptoms of the disease, further worsening their psychological impact.94
Coordination of Care for Patients With Psoriasis
It is essential that medical providers address the mental health comorbidities of patients with psoriasis. Unfortunately, depression symptoms in patients with psoriasis often go unrecognized or are inadequately treated.95 Comprehensive treatment, including mental health screenings, might lead to cost savings and benefitpatients.77 In general, European clinicians have greater awareness of the mental health burden of patients with psoriasis compared with their American colleagues. Europeans researchers have performed a number of scientific investigations of the topic.19,20,94,96-99
Various European guidelines have also moved to incorporate health-related QoL as part of general clinical assessment.95
Patients with psoriasis may benefit from specialist coordination of care to address their overall mental, emotional, and physical health.91 Patients with comorbid mental health disorders may particularly benefit from such integrated systems of care.99 When integrated multispecialty support is not available, the treating physicians must attempt to care of all aspects of a patient’s QoL.93 Providers must consider the primary symptoms of psoriasis and its potential cardiovascular and mental health comorbidities.
Many patients with psoriasis do not have their CV risk factors adequately assessed or managed. One study reported that approximately 20% of patients with moderate to severe psoriasis had undiagnosed hypertension, diabetes, or hypercholesterolemia. Moreover, 40% to 60% of patients were found not to be optimally managed for these conditions.100 Screening patients with psoriasis for such risk factors helps to identify a high proportion of individuals with potentially modifiable risk factors for CVD.101
Without multispecialty support, dermatologists may feel inadequately trained to address the mental health morbidities of the disease.93 Dermatologists must learn to screen for such problems and refer patients to psychiatrists or other mental health professionals when needed.93 Because of the increased risk of suicide, it is also essential that dermatologists screen for prior history of suicidal thoughts or present suicidality, especially in patients with severe disease.23
Many patients will need input from psychiatrists or psychologists as part of their care. Management of psycho-dermatological conditions, such as psoriasis requires that providers assess the social, familial, and occupational aspects of the condition.36 A variety of techniques are available to practitioners. For example, one study of 40 patients with psoriasis in Italy found that cognitive behavioral therapy combined with biofeedback improved PASI scores, QoL, and reduced the number of minor psychiatric disorders.98 Other prospective randomized trials’ findings have demonstrated that cognitive-behavioral approaches may be able to reduce psoriasis severity.98
Primary health providers can play a key role in care coordination. They may give support for the psychological aspects of psoriasis via referral to patient support groups, stress reduction therapy, psychologist or psychiatrist referral, or administration of psychotropic medications.36 Primary health providers should also be aware of the need for assessing cardiovascular risk factors in these patients.100
Managed health providers are also needed to help ensure that patients get access to the most appropriate treatments for them. Such cost/benefit calculations must consider the varying direct costs of treatment options. However, they must also weigh the costs of AEs, decreased work productivity, and inadequately treated disease and disease morbidities on the overall economic burden.102 At this time, we lack good data on many of these outcomes, and high-quality studies of long-term cost effectiveness are needed to help inform decision making.102
Conclusion
Psoriasis is a source of significant psychological strain and physical discomfort for patients.2 Treatment goals in the management of psoriasis continue to emerge. With the availability of newer and more effective treatments, researchers and clinicians are beginning to use higher standards to assess patient’s therapeutic goals.44 Direct and indirect financial and personal costs of the disease are quite substantial both for individuals and for society as a whole.32 Many of these costs result from the commonly associated disease comorbidities, which include CVD, obesity, PsA, and psychiatric disorders such as depression, which exert considerable personal and financial strain on society.2,32 Yet some practitioners continue to underestimate the severity and prevalence of mental health comorbidities.95 Managed care providers also need to incorporate updated criteria to provide more comprehensive analyses of the full impacts of psoriasis-related costs.31
Over time, we will gain a better understanding of how best to address the needs of patients with psoriasis in terms of their physical, emotional, and mental health.Author affiliations: Department of Dermatology, Kaiser Permanente Los Angeles Medical Center, Los Angeles, CA.
Funding source: This publication was sponsored by Ortho Dermatologics.
Author disclosures: Dr Wu reports serving as an investigator for and receiving grants from AbbVie, Inc; Amgen, Inc; Eli Lilly and Company; Janssen Pharmaceutical; Novartis International AG; and Regeneron Pharmaceuticals, Inc.
Authorship information: Concept and design; analysis and interpretation of data; critical revision of the manuscript for important intellectual content; administrative, technical or logistic support; and supervision.
Address correspondence to: E-mail: jashinwu@gmail.com
- Menter A, Gottlieb A, Feldman SR, , et al. Guidelines of care for the management of psoriasis and psoriatic arthritis: Section Overview of psoriasis and guidelines of care for the treatment of psoriasis with biologics. J Am Acad Dermatol. 2008;58(5):826-850.
- Menter A, Korman NJ, et al. Guidelines of care for the management of psoriasis and psoriatic arthritis: section 6. Guidelines of care for the treatment of psoriasis and psoriatic arthritis: case-based presentations and evidence-based conclusions. J Am Acad Dermatol. 2011;65(1):137-174.
- Rachakonda TD, Schupp CW, Armstrong AW. Psoriasis prevalence among adults in the United States. J Am Acad Dermatol. 2014;70(3):512-516. doi: 10.1016/j.jaad.20111.013.
- Armstrong AW. Psoriasis. JAMA Dermatol. 2017;153(9):956. doi: 10.1001/jamadermatol.2017.2103
- Wu JJ, No DJ, Amin M. BSA75, BSA90, and BSA100: new clinical tools for measuring improvement in psoriasis. Cutis. 2017;99(6):418.
- Armstrong AW, Siegel MP, Bagel J, et al. From the Medical Board of the National Psoriasis Foundation: Treatment targets for plaque psoriasis. J Am Acad Dermatol. 2017;76(2):290-298. doi: 10.1016/j.jaad.20110.017.
- Armstrong AW, Robertson AD, Wu J, Schupp C, Lebwohl MG. Undertreatment, treatment trends, and treatment dissatisfaction among patients with psoriasis and psoriatic arthritis in the United States: findings from the National Psoriasis Foundation surveys, 2003-2011. JAMA Dermatol. 2013;149(10):1180-1185. doi: 10.1001/jamadermatol.2013.5264.
- Carvalho AV, Romiti R, Souza CD, Paschoal RS, Milman LM, Meneghello LP. Psoriasis comorbidities: complications and benefits of immunobiological treatment. An Bras Dermatol. 2016;91(6):781-789. doi: 10.1590/abd1806-4841.20165080.
- Furue M, Tsuji G, Chiba T, Kadono T. Cardiovascular and metabolic diseases comorbid with psoriasis: beyond the skin. Intern Med. 2017;56(13):1613-161 doi:10.2169/internalmedicine.56.8209.
- Kimball AB, Robinson D Jr, Wu Y, et al. Cardiovascular disease and risk factors among psoriasis patients in two US healthcare databases, 2001-2002. Dermatology.2008;217(1):27-37. doi: 10.1159/000121333.
- Neimann AL, Shin DB, Wang X, Margolis DJ, Troxel AB, Gelfand JM. Prevalence of cardiovascular risk factors in patients with psoriasis. J Am Acad Dermatol. 2006;55(5):829-835. doi:10.1016/j.jaad.2006.08.040.
- Armstrong EJ, Harskamp CT, Armstrong AW. Psoriasis and major adverse cardiovascular events: a systematic review and meta-analysis of observational studies. J Am Heart Assoc. 2013;2(2):e000062. doi: 10.1161/JAHA.113.000062.
- Noe MH, Shin DB, Wan MT, Gelfand JM. Objective measures of psoriasis severity predict mortality: a prospective population-based cohort study. J Invest Dermatol. 2017. doi: 10.1016/j.jid.2017.07.841.
- Bremmer S, Van Voorhees AS, Hsu S, et al. Obesity and psoriasis: from the Medical Board of the National Psoriasis Foundation. J Am Acad Dermatol.2010;63(6):1058-1069. doi: 10.1016/j.jaad.2009.09.053.
- Armstrong AW, Harskamp CT, Armstrong EJ. The association between psoriasis and obesity: a systematic review and meta-analysis of observational studies. Nutr Diabetes. 2012;2:e54. doi: 10.1038/nutd.2012.26.
- Wee CC, Davis RB, Huskey KW, Jones DB, Hamel MB. QoL among obese patients seeking weight loss surgery: the importance of obesity-related social stigma and functional status. J Gen Intern Med. 2013;28(2):231-238. doi:10.1007/s11606-012-2188-0.
- Qureshi AA, Choi HK, Setty AR, Curhan GC. Psoriasis and the risk of diabetes and hypertension: a prospective study of US female nurses. Arch Dermatol. 2009;145(4):379-382. doi: 10.1001/archdermatol.2009.48.
- Kerschbaumer A, Fenzl KH, Erlacher L, Aletaha D. An overview of psoriatic arthritis - epidemiology, clinical features, pathophysiology and novel treatment targets. Wien Klin Wochenschr. 2016;128(21-22):791-795. doi: 10.1007/s00508-016-1111-9.
- Dowlatshahi EA, Wakkee M, Arends LR, Nijsten T. The prevalence and odds of depressive symptoms and clinical depression in psoriasis patients: a systematic review and meta-analysis. J Invest Dermatol. 2014;134(6):1542-1551. doi : 10.1038/jid.2013.508.
- Dominguez P, Han J, Li T, Ascherio A, Qureshi A. Depression and the risk of psoriasis in US women. J Eur Acad Dermatol Venereol. 2013;27(9):1163-1167. doi: 10.1111/j.1468-3083.2012.04703.x.
- Connor CJ, Liu V, Fiedorowicz JG. Exploring the physiological link between psoriasis and mood disorders. Dermatol Res Pract. 2015;2015:409637. doi: 10.1155/2015/409637.
- Hayes J, Koo J. Psoriasis: depression, anxiety, smoking, and drinking habits. Dermatol Ther. 2010;23(2):174-180. doi: 10.1111/j.1529-8019.2010.01312.x.
- Singh S, Taylor C, Kornmehl H, Armstrong AW. Psoriasis and suicidality: A systematic review and meta-analysis. J Am Acad Dermatol. 2017;77(3):425-440.e2. doi: 10.1016/j.jaad.2017.05.019.
- Bhosle MJ, Kulkarni A, Feldman SR, Balkrishnan R. QoL in patients with psoriasis. Health Qual Life Outcomes. 2006;4:35. doi: 10.1186/1477-7525-4-35.
- Dunbar JA, Reddy P, Davis-Lameloise N, et al. Depression: An important comorbidity with metabolic syndrome in a general population. Diabetes Care. 2008;31(12):2368-2373. doi:10.2337/dc08-0175.
- Egede LE. Major depression in individuals with chronic medical disorders: prevalence, correlates and association with health resource utilization, lost productivity and functional disability. Gen Hosp Psychiatry. 2007;29(5):409-416.
- Husni ME, Merola JF, Davin S. The psychosocial burden of psoriatic arthritis. Semin Arthritis Rheum. 2017;47(3):351-360. doi: 10.1016/j.semarthrit.2017.05.010.
- Dommasch ED, Li T, Okereke OI, et al. Risk of depression in women with psoriasis: a cohort study. Br J Dermatol. 2015;173(4):975-980. doi:10.1111/bjd.14032.
- Wu JJ, Penfold RB, Primatesta P, et al. The risk of depression, suicidal ideation and suicide attempt in patients with psoriasis, psoriatic arthritis or ankylosing spondylitis. J Eur Acad Dermatol Venereol. 2017;31(7):1168-1175. doi: 10.1111/jdv.14175.
- Lewinson RT, Vallerand IA, Lowerison MW, et al. Depression Is associated with an increased risk of psoriatic arthritis among patients with psoriasis: a population-based study. J Invest Dermatol. 2017;137(4):828-835. doi: 10.1016/j.jid.2016.11.032.
- Evans C. Managed care aspects of psoriasis and psoriatic arthritis. Am J Manag Care. 2016;22(suppl 8):s238-s243.
- Brezinski EA, Dhillon JS, Armstrong AW. Economic burden of psoriasis in the United States: a systematic review. JAMA Dermatol. 2015;151(6):651-658. doi: 10.1001/jamadermatol.2014.3593.
- Armstrong AW, Zhao Y, Herrera V, Li Y, Bancroft T, Hull M, Altan A. Drivers of healthcare costs among the costliest patients with psoriasis over three years in a United States health plan. J Drugs Dermatol. 2017;16(7):651-658.
- Feldman SR, Tian H, Gilloteau I, Mollon P, Shu M. Economic burden of comorbidities in psoriasis patients in the United States: results from a retrospective U.S. database. BMC Health Serv Res. 2017;17(1):337. doi: 10.1186/s12913-017-2278-0.
- Korman NJ, Zhao Y, Pike J, Roberts J. Relationship between psoriasis severity, clinical symptoms, QoL and work productivity among patients in the USA. Clin Exp Dermatol. 2016;41(5):514-521. doi: 10.1111/ced.12841.
- Koo J, Lebwohl A. Psycho dermatology: the mind and skin connection. Am Fam Physician. 2001;64(11):1873-1878.
- Armstrong AW, Schupp C, Wu J, Bebo B. QoL and work productivity impairment among psoriasis patients: findings from the National Psoriasis Foundation survey data 2003-2011. PloS One. 2012;7(12):e52935-e52011. doi: 10.1371/journal.pone.0052935.
- Spuls PI, Lecluse LL, Poulsen ML, Bos JD, Stern RS, Nijsten T. How good are clinical severity and outcome measures for psoriasis?: quantitative evaluation in a systematic review. J Invest Dermatol. 2010;130(4):933-943. doi: 10.1038/jid.2009.391.
- Feldman SR, Krueger GG. Psoriasis assessment tools in clinical trials. Ann Rheum Dis. 2005;64 (Suppl 2):ii65-ii68; discussion ii69-ii73. doi: 10.1136/ard.2004.031237.
- Puig L. PASI 90 response: the new standard in therapeutic efficacy for psoriasis. J Eur Acad Dermatol Venereol. 2015;29(4):645-648. doi: 10.1111/jdv.12817.
- Ahn CS, Gustafson CJ, Sandoval LF, Davis SA, Feldman SR. Cost effectiveness of biologic therapies for plaque psoriasis. Am J Clin Dermatol. 2013;14(4):315-326. doi: 10.1007/s40257-013-0030-z.
- Duffin KC, Papp KA, Bagel J, et al. Evaluation of the Physician Global Assessment and Body Surface Area Composite Tool for assessing psoriasis response to apremilast therapy: results from ESTEEM 1 and ESTEEM 2. J Drugs Dermatol. 2017;16(2):147-153.
- Menter A, Korman NJ, Elmets CA, et al. Guidelines of care for the management of psoriasis and psoriatic arthritis. Section 3. Guidelines of care for the management and treatment of psoriasis with topical therapies. J Am Acad Dermatol. 2009;60(4):643-659. doi: 10.1016/j.jaad.2008.12.032
- Menter A, Korman NJ, Elmets CA, et al. Guidelines of care for the management of psoriasis and psoriatic arthritis: section 4. Guidelines of care for the management and treatment of psoriasis with traditional systemic agents. J Am Acad Dermatol. 2009;61(3):451-485.
- Manalo IF, Gilbert KE, Wu JJ. Time to raise the bar to Psoriasis Area Severity Index 90 and 100. J Drugs Dermatol. 2015;14(10):1086-1088.
- Gu T, Shah N, Deshpande G, Tang DH, Eisenberg DF. Comparing biologic cost per treated patient across indications among adult US managed care patients: a retrospective cohort study. Drugs Real World Outcomes. 2016;3(4):369-381. doi: 10.1007/s40801-016-0093-2.
- Otelza [package insert]. Summit, New Jersey: Celgene Corporation; 2014.
- Papp K, Reich K, Leonardi CL, et al. Apremilast, an oral phosphodiesterase 4 (PDE4) inhibitor, in patients with moderate to severe plaque psoriasis: Results of a phase III, randomized, controlled trial (Efficacy and Safety Trial Evaluating the Effects of Apremilast in Psoriasis [ESTEEM] 1). J Am Acad Dermatol. 2015;73(1):37-49. doi: 10.1016/j.jaad.2015.03.049.
- Feldman SR, Goffe B, Rice G, et al. The challenge of managing psoriasis: unmet medical needs and stakeholder perspectives. Am Health Drug Benefits. 2016;9(9):504-513.
- Ekelund M, Mallbris L, Qvitzau S, Stenberg B. A higher score on the dermatology life quality index, being on systemic treatment and having a diagnosis of psoriatic arthritis is associated with increased costs in patients with plaque psoriasis. Acta Derm Venereol. 2013;93(6):684-688. doi: 10.2340/00015555-1591.
- Strober B, Papp KA, Lebwohl M, et al. Clinical meaningfulness of complete skin clearance in psoriasis. J Am Acad Dermatol. 2016;75(1):77-82.e7. doi: 10.1016/j.jaad.2016.03.026.
- Leonardi CL, Kimball AB, Papp KA, et al. Efficacy and safety of ustekinumab, a human interleukin-12/23 monoclonal antibody, in patients with psoriasis: 76-week results from a randomized, double-blind, placebo-controlled trial (PHOENIX 1). Lancet. 2008;371(9625):1665-1674. doi: 10.1016/S0140-6736(08)60725-4.
- Leonardi CL, Powers JL, Matheson RT, et al; Etanercept Psoriasis Study Group. Etanercept as monotherapy in patients with psoriasis. N Engl J Med. 2003;349(21):2014-2022.
- Reich K, Nestle FO, Papp K, et al. Infliximab induction and maintenance therapy for moderate-to-severe psoriasis: a phase III, multicentre, double-blind trial. Lancet. 2005;366(9494):1367-1374.
- Gordon KB, Blauvelt A, Papp KA, et al; UNCOVER-1 Study Group; UNCOVER-2 Study Group; UNCOVER-2 Study Group. Phase 3 trials of ixekizumab in moderate-to-severe plaque psoriasis. N Engl J Med. 2016;375(4):345-356. doi: 10.1056/NEJMoa1512711.
- Reich K, Papp KA, Blauvelt A, et al. Tildrakizumab versus placebo or etanercept for chronic plaque psoriasis (reSURFACE 1 and reSURFACE 2): results from two randomised controlled, phase 3 trials. Lancet. 2017;390(10091):276-288. doi: 10.1016/S0140-6736(17)31279-5.
- Langley RG, Elewski BE, Lebwohl M, et al. Secukinumab in plaque psoriasis—results of two phase 3 trials. N Engl J Med. 2014;371(4):326-338. doi: 10.1056/NEJMoa1314258.
- Lønnberg AS, Zachariae C, Skov L. Targeting of interleukin-17 in the treatment of psoriasis. Clin Cosmet Investig Dermatol.. 2014;7:251-259. doi: 10.2147/CCID.S67534.
- Reich K, Armstrong AW, Foley P, et al. Efficacy and safety of guselkumab, an anti-interleukin-23 monoclonal antibody, compared with adalimumab for the treatment of patients with moderate to severe psoriasis with randomized withdrawal and retreatment: Results from the phase III, double-blind, placebo- and active comparator-controlled VOYAGE 2 trial. J Am Acad Dermatol. 2017;76(3):418-431. doi: 10.1016/j.jaad.2016.11.042.
- Blauvelt A, Papp KA, Griffiths CE, et al. Efficacy and safety of guselkumab, an anti-interleukin-23 monoclonal antibody, compared with adalimumab for the continuous treatment of patients with moderate to severe psoriasis: Results from the phase III, double-blinded, placebo- and active comparator-controlled VOYAGE 1 trial. J Am Acad Dermatol. 2017;76(3):405-423. doi: 10.1016/j.jaad.2016.11.041.
- Papp KA, Blauvelt A, Bukhalo M, et al. Risankizumab versus ustekinumab for moderate-to-severe plaque psoriasis. N Engl J Med. 2017;376(16):1551-1560. doi: 10.1056/NEJMoa1607017.
- Griffiths CE, Reich K, Lebwohl M, et al. Comparison of ixekizumab with etanercept or placebo in moderate-to-severe psoriasis (UNCOVER-2 and UNCOVER-3): results from two phase 3 randomised trials. Lancet. 2015;386(9993):541-551. doi: 10.1016/S0140-6736(15)60125-8.
- Papp KA, Reich K, Paul C, et al. A prospective phase III, randomized, double-blind, placebo-controlled study of brodalumab in patients with moderate-to-severe plaque psoriasis. Br J Dermatol. 201;175(2):273-286. doi: 10.1111/bjd.14493.
- Lebwohl M, Strober B, Menter A, et al. Phase 3 studies comparing brodalumab with ustekinumab in psoriasis. N Engl J Med. 2015;373(14):1318-1328. doi: 10.1056/NEJMoa1503824.
- Enbrel [package insert]. Thousand Oaks, CA: Amgen; 2017.
- Remicade [package insert]. Horsham, PA: Janssen Biotech, Inc; 2013.
- Humira [package insert]. North Chicago, IL: AbbVie Inc; 2017.
- Menter A, Tyring SK, Gordon K, et al. Adalimumab therapy for moderate to severe psoriasis: A randomized, controlled phase III trial. J Am Acad Dermatol. 2008;58(1):106-115.
- Stelara [package insert]. Thousand Oaks, CA: Janssen Biotech, Inc; 2014.
- Papp KA, Langley RG, Lebwohl M, et al; PHOENIX 2 study investigators. Efficacy and safety of ustekinumab, a human interleukin-12/23 monoclonal antibody, in patients with psoriasis: 52-week results from a andomized, double-blind, placebo-controlled trial (PHOENIX 2). Lancet. 2008;371(9625):1675-1684. doi: 10.1016/S0140-6736(08)60726-6.
- Cosentyx [package insert]. East Hanover, NJ: Novartis Pharmaceutical Corporation; 2017.
- Taltz [package insert]. Indianapolis, IN: Eli Lilly and Company; 2017.
- Siliq [package insert]. Bridgewater, NJ: Valeant Pharmaceuticals; 2017.
- Tremfya [package insert]. Horsham, PA: Janssen Biotech, Inc; 2017.
- Menter A, Thaçi D, Wu JJ, et al. Long-term safety and effectiveness of adalimumab for moderate to severe psoriasis: results from 7-year interim analysis of the ESPRIT Registry. Dermatology and Therapy. 2017;7(3):365-381. doi:10.1007/s13555-017-0198-x.
- Tyring S, Gottlieb A, Papp K, et al. Etanercept and clinical outcomes, fatigue, and depression in psoriasis: double-blind placebo-controlled randomized phase III trial. Lancet. 2006;367(9504):29-35.
- Menter A, Augustin M, Signorovitch J, et al. The effect of adalimumab on reducing depression symptoms in patients with moderate to severe psoriasis: a randomized clinical trial. J Am Acad Dermatol. 2010;62(5):812-818. doi: 10.1016/j.jaad.2009.07.022.
- Amjevita [package insert]. Thousand Oaks, CA: Amgen Inc; 2016.
- Cyltezo [package insert]. Ridgefield, CT: Boehringer Ingelheim Pharmaceuticals, Inc.;2017.
- Erelzi [package insert]. Princeton, NJ: Sandoz Inc; 2016.
- Inflectra [package insert]. Incheon, Republic of Korea: Celltrion, Inc; 2016.
- Renflexis [package insert]. Kenilworth, NJ: Merck & Co. Inc; 2017.
- Langley RG, Feldman SR, Han C, et al. Ustekinumab significantly improves symptoms of anxiety, depression, and skin-related QoL in patients with moderate-to-severe psoriasis: Results from a randomized, double-blind, placebo-controlled phase III trial. J Am Acad Dermatol. 2010;63(3):457-65. Doi: 10.1016/j.jaad.2009.09.014.
- Center for Drug Evaluation and Research. Summary Review. [Brodalumab]. 2017.
- Lebwohl MG, Papp KA, Marangell LB, et al. Psychiatric adverse events during treatment with brodalumab: analysis of psoriasis clinical trials. J Am Acad Dermatol. 2017;S0190-9622(17)32256-32259. doi:10.1016/j.jaad.2017.08.024.
- A study of ixekizumab (LY2439821) in participants with moderate-to-severe plaque psoriasis naive to systemic treatment. clinicaltrials.gov/ct2/show/NCT02634801. Updated December 4, 2017. Accessed August 24, 2017.
- A study of KHK4827 (brodalumab) in subjects with moderate to severe psoriasis in Korea. clinicaltrials.gov/ct2/show/NCT02982005. Updated June 8, 2017. Accessed August 24, 2017.
- Wu JJ, Feldman SR, Koo L, et al. Epidemiology of mental health comorbidity in psoriasis [published online November 10, 2017]. J Dermatolog Treat. 2017;1-9. doi: 10.1080/09546634.2017.1395800.
- BI 655066 (risankizumab) compared to placebo and active comparator (ustekiinumab) in patients with moderate to severe chronic plaque psoriasis. clinicaltrials.gov/ct2/show/NCT02684370. Updated December 5, 2017. Accessed November 13, 2017.
- BI 655066 (risankizumab) compared to placebo and active comparator (ustekiinumab) in patients with moderate to severe chronic plaque psoriasis. clinicaltrials.gov/ct2/show/NCT02684357. Updated December 5, 2017. Accessed November 13, 2017.
- Basavaraj KH, Navya MA, Rashmi R. Relevance of psychiatry in dermatology: present concepts. Indian J Psychiatry. 2010;52(3):270-275. doi:10.4103/0019-5545.70992.
- Stern RS, Nijsten T, Feldman SR, et al. Psoriasis is common, carries a substantial burden even when not extensive, and is associated with widespread treatment dissatisfaction. J Investig Dermatol Symp Proc. 2004;9(2):136-139.
- Connor CJ. Management of the psychological comorbidities of dermatological conditions: practitioners’ guidelines. Clin Cosmet Investig Dermatol. 2017;10:117-132. doi: 10.2147/CCID.S111041.
- Ferreira BI, Abreu JL, Reis JP, Figueiredo AM. Psoriasis and associated psychiatric disorders: a systematic review on etiopathogenesis and clinical correlation. J Clin Aesthet Dermatol. 2016;9(6):36-43.
- Moon HS, Mizara A, McBride SR. Psoriasis and psycho-dermatology. Dermatology and Therapy. 2013;3(2):117-130. doi: 10.1007/s13555-013-0031-0.
- Dalgard FJ, Gieler U, Tomas-Aragones L, et al. The psychological burden of skin diseases: a cross-sectional multicenter study among dermatological out-patients in 13 European countries.J Invest Dermatol. 2015;135(4):984-991. doi: 10.1038/jid.2014.530.
- Owczarek K, Jaworski M. QoL and severity of skin changes in the dynamics of psoriasis. Postepy Dermatol Alergol. 2016;33(2):102-108. doi: 10.5114/pdia.2015.54873.
- Piaserico S, Marinello E, Dessi A, Linder MD, Coccarielli D, Peserico A. efficacy of biofeedback and cognitive-behavioral therapy in psoriatic patients A single-blind, randomized and controlled study with added narrow-band ultraviolet B therapy. Acta Derm Venereol. 2016;96(217):91-95. doi: 10.2340/00015555-2428.
- Schmitt J, Wozel G, Garzarolli M, Viehweg A, Bauer M, Leopold K. Effectiveness of interdisciplinary vs. dermatological care of moderate-to-severe psoriasis: a pragmatic andomized controlled trial. Acta Derm Venereol. 2014;94(2):192-197. doi: 10.2340/00015555-1697.
- Kimball AB, Szapary P, Mrowietz U, et al. Underdiagnosis and undertreatment of cardiovascular risk factors in patients with moderate to severe psoriasis. J Am Acad Dermatol. 2012;67(1):76-85. doi: 10.1016/j.jaad.2011.06.035.
- Rutter MK, Kane K, et al. Primary care-based screening for cardiovascular risk factors in patients with psoriasis. Br J Dermatol. 2016;175(2):348-356. doi: 10.1111/bjd.14557.
- Zhang W, Islam N, Ma C, Anis AH. Systematic review of cost-effectiveness analyses of treatments for psoriasis. Pharmacoeconomics. 2015;33(4):327- 40. doi: 10.1007/s40273-014-0244-9.
Articles in this issue
Newsletter
Stay ahead of policy, cost, and value—subscribe to AJMC for expert insights at the intersection of clinical care and health economics.