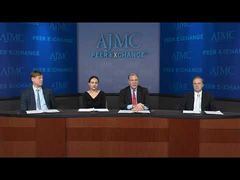
Therapies in the Pipeline for HIV
Episodes in this series
William Short, MD, MPH, AAHIVS: Again, looking through the evolution of antiretrovirals, we started out with a single drug in 1987, AZT. And then we sort of followed that with dual therapy. And in 1996, we got to an era where we said, “All right, this is where you need to use 3 drugs.” And that sort of set the stage moving forward for success. With that success then came refining all the things we knew, making the drugs better, and then trying to make them simpler, getting them into single-tablet regimens.
So where we’re going now in the field is, and we’ve seen a little bit this year for the first time, we had the first in a new treatment paradigm. From 1996, the standard of care has been using 3 drugs to treat HIV. For the first time this year, we have approval of our first 2-drug regimen, eliminating one of the components. And this place, what was approved now, it was the NRTI, so the nucleoside reverse transcriptase inhibitors. Why those? Well, we know those are the ones associated with a lot of toxicity. So we talked about Truvada. Truvada in long-term use can cause kidney damage, bone damage. So it’s really eliminating those. And so that’s been sort of, really a paradigm shift for us, because every one of us is used to 3 drugs.
Concerns around using 2 drugs include using the regimen in patients who are poorly adherent to drugs. Do they have background resistance? And will 2 drugs be enough? I think when you look back, when you go back to 1991 when DVI was approved, those 2 drugs were very different than what we’re looking at now. Those drugs were not the best drugs, whereas the true drugs we now have in a single pill really are good drugs. So, again, one combination approved, another one to follow, and then really right behind that is, again, a whole new treatment paradigm for us, and that’s using injectables in depot forms.
So patients will come in once a month, get a depot shot, and again, it’s going to be of 2 drugs. We’re hoping, to be approved, cabotegravir, which is an integrase inhibitor, and rilpivirine, a non-nucleoside reverse transcriptase inhibitor, where they would get injections once a month in a depot form and they would not have to take pills. And the studies that are out there really look well in terms of success rate, so we’re really looking forward to those times. And patients are really looking forward to this. There are many patients who cannot tolerate pills. Many patients don’t want to take a pill once a day. For some patients, it’s a reminder of their HIV status. So to be able to come in and get a single injection once a month will really be exciting.
The guidelines, I anticipate—and actually with the latest iteration, one of the new single-drug combos, dolutegravir with lamivudine, was already added as an agent on there and it’s not even approved yet. So I think knowing that these drugs are really efficacious, they’re very well tolerated, the guidelines, I feel, will have no problem putting them up there as first-line agents.
I don’t know that they’re going to be first-line treatment for everyone. You know the guidelines sort of break it up as to what drugs are best for every one of them, what drugs are best for certain key populations, and we do know that when we’re using 2-drug combinations they are not for everyone. They are not for someone in whom you’re worried about adherence. They are not for someone for whom you’re worried about resistance. So I think they will put that there, but I do think they will move them up pretty rapidly.























