News
Article
Data on Delandistrogene Moxeparvovec Can Inform Future Gene Therapies
Author(s):
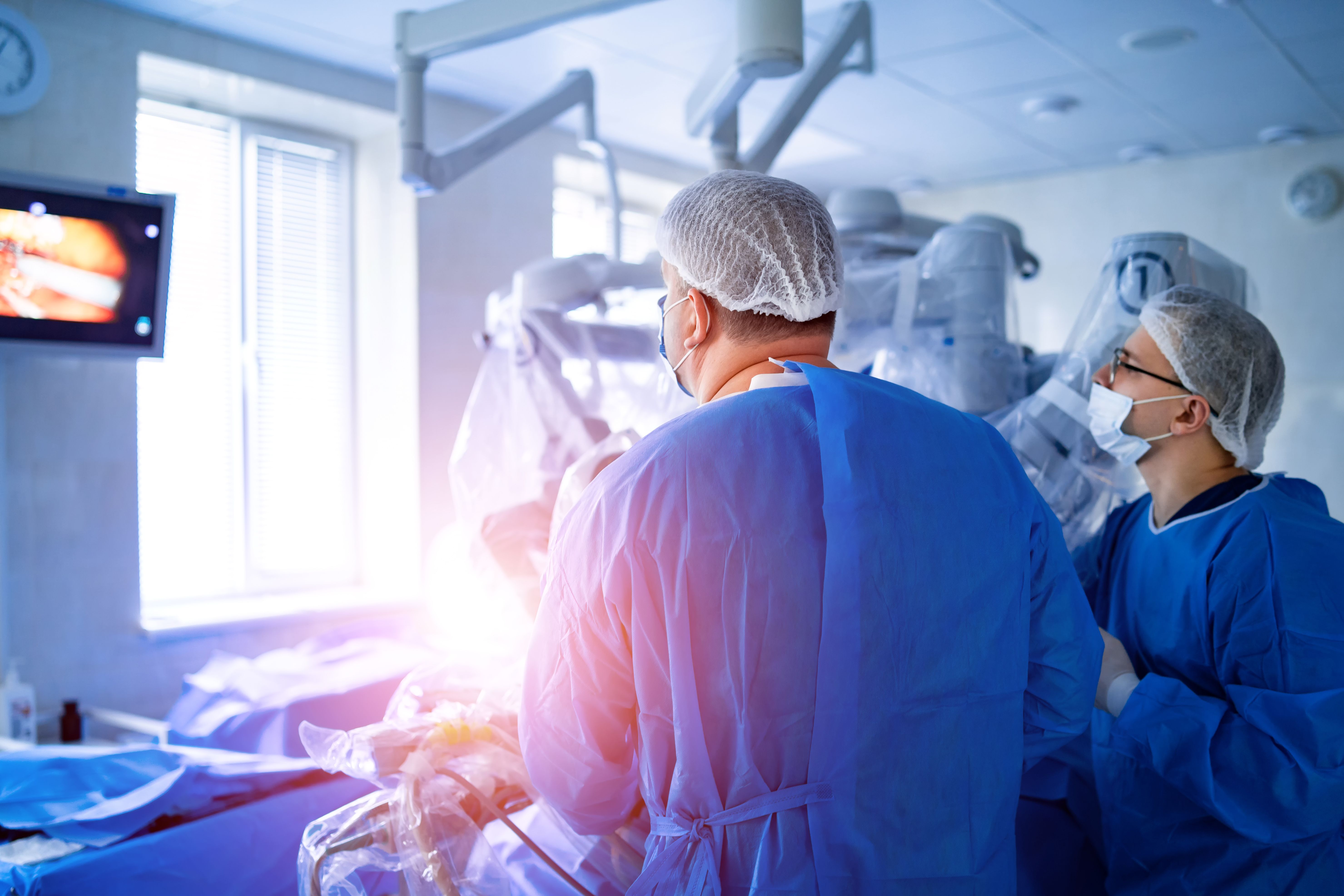
The FDA approved delandistrogene moxeparvovec-rokl (Elevidys, Sarepta Therapeutics) in June to treat Duchenne muscular dystrophy in ambulatory pediatric patients aged 4 through 5 who have a confirmed DMD gene mutation.
Scientific spillover from delandistrogene moxeparvovec (Elevidys, Sarepta Therapeutics) has potential to reverberate across preclinical studies, patient populations, treatment efficacy, safety monitoring, and manufacturing processes, influencing and accelerating the development of future gene therapies, according to research published in Molecular Therapy: Methods & Clinical Development.1
The FDA approved delandistrogene moxeparvovec in June to treat Duchenne muscular dystrophy (DMD) in ambulatory pediatric patients aged 4 through 5 who have a confirmed DMD gene mutation; dosing is based on patient weight.
DNA molecules | Image Credit: vitstudio - stock.adobe.com

“Gene therapy advancement requires extensive development at each stage: preclinical work to create and evaluate vehicles for delivery of the therapy, design of clinical development programs, and establishment of a large-scale manufacturing process,” study authors wrote. “Consequently, the benefits of these therapies extend beyond offering knowledge for treating any one disease to establishing new platforms and paradigms that will accelerate advancement of future gene therapies.”
In particular, scientific spillover is important in the rare disease space because it has potential to shorten development time and lower treatment cost. DMD is considered a rare muscle disorder despite being one of the most frequently diagnosed genetic conditions,2 so the study authors used delandistrogene moxeparvovec as a case study for scientific spillover.
Preclinical Studies
In DMD, mutations in the DMD gene are known to affect production of the dystrophin protein, which plays an important role in muscle cell membrane maintenance. The transgene engineering used to construct delandistrogene moxeparvovec allows it to retain key anchoring regions that help it to produce functioning dystrophin. This “construct optimization,” according to the study authors, can be applied to thousands of monogenic diseases caused by genes that exceed the packaging capacity of the adeno-associated virus (AAV) vehicles often used to deliver gene therapies.
Patient Populations
The study investigators stressed the importance of referring to previous research in the same field to help select the patient populations best suited for initial clinical trials of new therapies. For example, based on the investigation of delandistrogene moxeparvovec in patients aged 4 to 7 years, which led to its approval, current studies are investigating the treatment in patients aged 8 to younger than 18 years and 3 to younger than 4 years,3 and 3 months to 3 years.4 Information on the safety and monitoring needs of future gene therapies can also be gleaned from delandistrogene moxeparvovec, because the therapy requires more viral vectors vs onasemnogene abeparvovec (used to treat spinal muscular atrophy) and voretigene neparvovec (used to treat retinal dystrophy); this can inform researchers on how to safely dose adjust both current and future gene therapies for older, heavier patients.
Efficacy and Safety
Stating that delandistrogene moxeparvovec is “currently the most advanced clinical program of systemic gene therapy for DMD,” the study investigators noted that for efficacy, other muscular dystrophy trials have used its data on measures of muscle function as benchmarks for disease inhibition and muscle functional recovery. Regarding safety, prophylactic and management protocols that managed off-target effects of the treatment (eg, vomiting, higher levels of transaminases) have been used to inform studies of limb girdle muscular dystrophy.
Manufacturing
Because delandistrogene moxeparvovec requires large-scale manufacturing due to its weight-based dosing and that it serves a larger patient population vs onasemnogene abeparvovec and voretigene neparvovec, advances in its manufacturing process “are also likely to result in scientific spillover for subsequent gene therapies,” the study authors wrote. For example, efficiency improvements that have led to greater therapy yields and lower cycle times have potential to decrease the costs to manufacture gene therapies. At present, the world’s most expensive drug is a gene therapy: Etranacogene dezaparvovec (Hemgenix, CSL Behring) costs $3.5 million for a 1-time infusion.5
“Gene therapy is an exciting new area of medical research and drug development that targets the root cause of a disease (i.e., at the genetic level),” the authors concluded. “Ultimately, scientific spillover provides value for the development of subsequent treatments, including for those targeted to treat rare diseases with high unmet needs; these potential benefits to society should be considered when evaluating the value of novel therapies.”
References
- Asher D, Dai D, Klimchak AC, Sedita LE, Gooch KL, Rodino-Klapac L. Paving the way for future gene therapies: A case study of scientific spillover from delandistrogene moxeparvovec. Mol Ther Methods Clin Dev. 2023;30:474-483. doi:10.1016/j.omtm.2023.08.002
- Duchenne muscular dystrophy. National Organization for Rare Disorders. Updated June 28, 2023. Accessed November 16, 2023. https://rarediseases.org/rare-diseases/duchenne-muscular-dystrophy/
- A gene transfer therapy study to evaluate the safety of and expression from delandistrogene moxeparvovec (srp-9001) in participants with Duchenne muscular dystrophy (DMD) (ENDEAVOR). Updated August 1, 2023. Accessed November 16, 2023. https://clinicaltrials.gov/study/NCT04626674
- A gene transfer therapy study to evaluate the safety of delandistrogene moxeparvovec (srp-9001) in participants with Duchenne muscular dystrophy (DMD). Updated August 1, 2023. Accessed November 16, 2023. https://clinicaltrials.gov/study/NCT03375164
- FDA approves first gene therapy to treat adults with hemophilia B. News release. FDA. November 22, 2022. Accessed November 16, 2023. https://www.fda.gov/news-events/press-announcements/fda-approves-first-gene-therapy-treat-adults-hemophilia-b
Newsletter
Stay ahead of policy, cost, and value—subscribe to AJMC for expert insights at the intersection of clinical care and health economics.