News
Article
Dry Eye Associated With Living Near Industrial Zones, Exposure to Sulfur Dioxide
Author(s):
Associations between ambient air pollutants and dry eye could have been mitigated during the pandemic.
Exposure to sulfur dioxide (SO2) and residence near industrial zones were found to be associated with dry eye symptoms (DES) during the COVID-19 pandemic, according to a study published in Science of the Total Environment.1 DES could also have been affected by the pandemic, when the population spent more time indoors.
DES is an eye disease characterized by film instability, pain, blurred vision, and burning sensation. DES are vital in determining a diagnosis of dry eye. Although the incidence of dry eye increased during the pandemic both globally2 and in populations of doctors and high school students in China, studies have not focused on the general population for these studies. This study aimed to estimate the prevalence of DES in China, explore if air pollution increased the risk of DES, and assess the relationship between air pollution and DES during the pandemic.
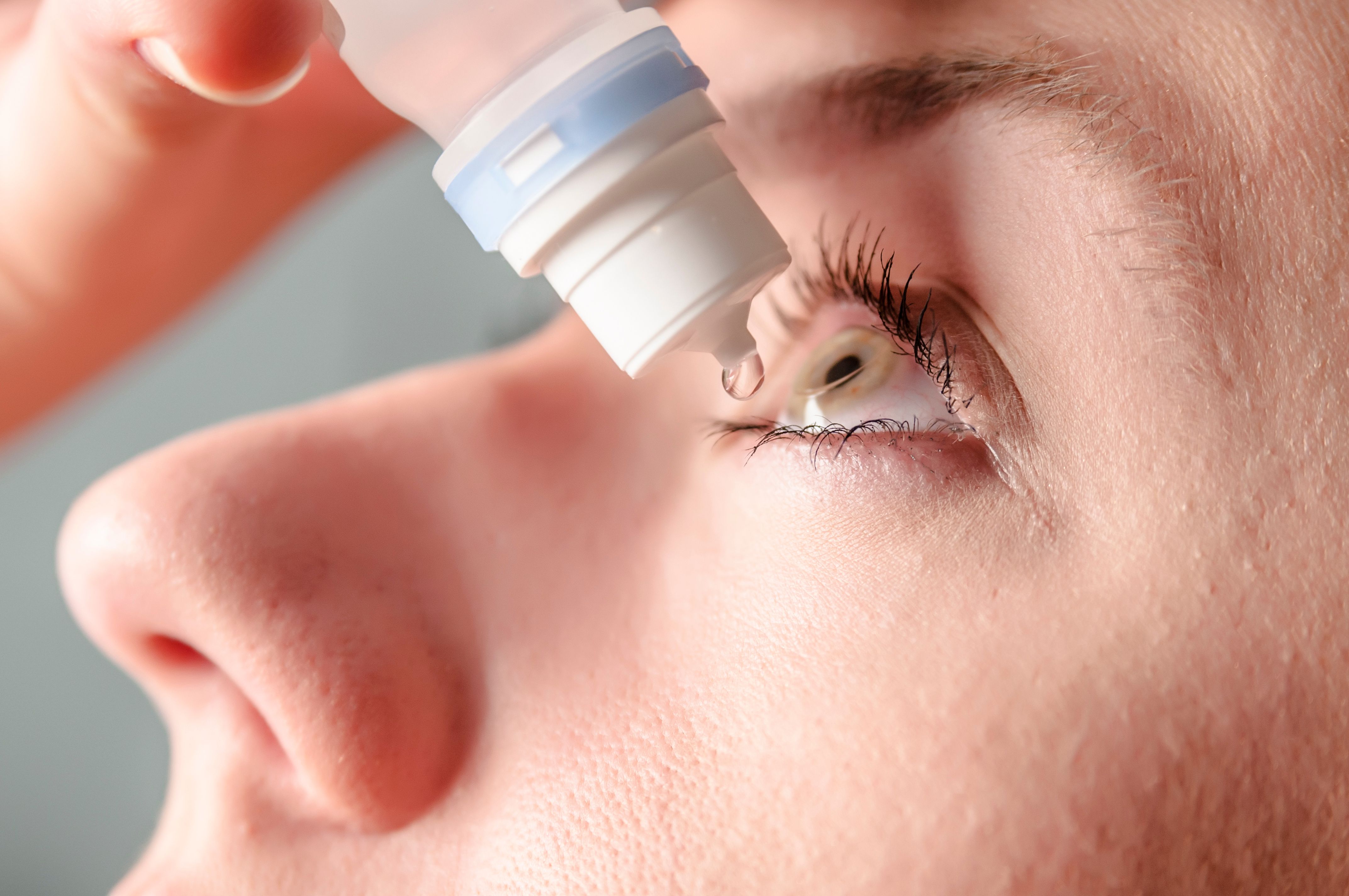
Woman applying eye drops to dry eyes | Image credit: Dragana Gordic - stock.adobe.com
A nationwide cross-sectional survey, the psychology and behavior investigation of Chinese residents, was used to collect data. This survey was conducted between June 20, 2022, and August 31, 2022. DES were measured using the Ocular Surface Disease Index-6, which consists of 3 subscales of ocular symptoms, vision-related function, and environmental factors. Air quality index (AQI), particulate matter 2.5. SO2, carbon monoxide, nitrogen dioxide, particulate matter 10, and ozone were also measured. Participants were also asked if they lived near industrial zones.
Data on sociodemographic factors and other covariates were collected at the start of the study. This included data on anxiety and depression of all participants.
There were 21,909 participants included in this study who had a mean (SD) age of 39.4 (18.8) years; 50% were women. The prevalence of DES was found to be 43.6% (95% CI, 43.0%-44.3%) during the pandemic, with more prevalence in women, adolescents, and older adults.
An increased risk of DES was only found in connection with SO2 (OR, 1.05; 95% CI, 1.02-1.09 per SD increment) in the logistic regression model. No other air pollutants had a similar association. Higher risk of DES was also correlated with residing near an industrial zone (OR, 1.57; 95% CI, 1.38-1.79). Depression had a correlation with DES (OR, 2.15; 95% CI, 1.82-2.54), but had a greater association when combined with SO2 exposure (OR, 2.50; 95% CI, 2.10-2.97), indicating a synergistic effect. The subgroup analysis found that the association between DES and SO2 was seen in participants who were older than 50 years (OR, 1.14; 95% CI, 1.08-1.21).
There were some limitations to this study. Objective examinations of dry eye were not conducted, which means DES alone cannot be considered a diagnosis of dry eye. Also, AQI was determined by averaging the air pollution data over 3 months, which may not be an accurate assessment of exposure. Further, use of eye drops and residential greenness were not controlled for this study and could have affected the results.
Exposure to SO2 and residing near an industrial zone were both found to be associated with an increased risk of DES, and depression could play a pronounced role in the development of DES. The pandemic could have affected associations to other air pollutants and further studies should be conducted to further confirm these findings, the study investigators concluded.
References
1. Kai JY, Wu YB, Dong XX, et al. Association between ambient air pollution and dry eye symptoms among Chinese individuals during the COVID-19 pandemic: a national-based study. Sci Total Environ. 2024;935:173386. doi:10.1016/j.scitotenv.2024.173386
2. Ji H, Yang Y, Lu Y, et al. Prevalence of dry eye during the COVID-19 pandemic: a systematic review and meta-analysis. PLoS One. 2023;18(12):e0288523. doi:10.1371/journal.pone.0288523
Newsletter
Stay ahead of policy, cost, and value—subscribe to AJMC for expert insights at the intersection of clinical care and health economics.