News
Article
Heart Study Shows Atrial Shunting Shrinks Left Side, Expands Right
Author(s):
Patients who responded positively to shunt treatment experienced more beneficial changes in their heart's structure and function compared with nonresponders.
After 2 years of follow-up, a post hoc analysis of the REDUCE LAP-HF II trial revealed that when there were holes in the upper chambers of the heart (atrial shunting), the left side of the heart got smaller while the right side got bigger, matching the flow of the shunt. However, there wasn't any change in how well the right ventricle pumped blood compared with a sham treatment.
Chambers of the heart | Image credit: melazerg – stock.adobe.com
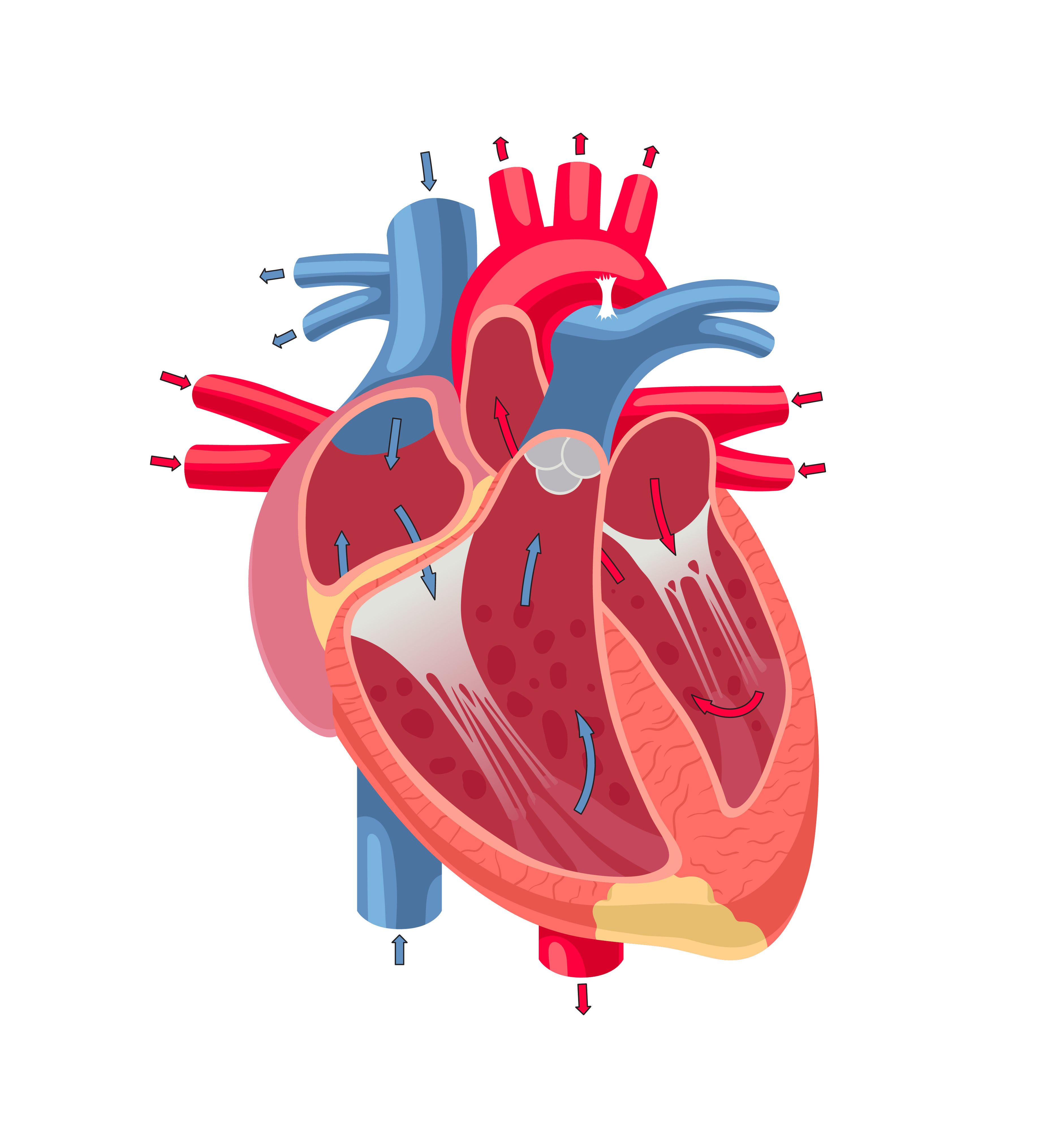
Cleveland Clinic defines a cardiac shunt as an irregular pattern of blood flow in the heart from one area—blood vessel or heart chamber—to another.1 A cardiac shunt can exist alongside or in place of typical blood flow patterns.
In patients who responded positively to shunt treatment, there were more beneficial changes in their heart's structure and function compared with nonresponders. This reinforces previous research that there might be certain groups of patients who respond better to this treatment, along with the proposed mechanism for why this happens. However, more research with longer follow-up periods is necessary to fully understand and confirm these findings.
These findings were published in JAMA Cardiology and are based on research of patients with heart failure with preserved ejection fraction (HFpEF) or with mildly reduced ejection fraction.2 Although the results of the REDUCE LAP-HF II trial were deemed neutral overall, the authors found that atrial shunt therapy had potential efficacy in responders, defined as patients without latent pulmonary vascular disease and who did not have a cardiac rhythm management device. In the current study, post hoc analyses were conducted over 2 years to assess the effect of shunt vs sham stratified by responder status. The researchers determined the effect based on changes in echocardiographic measures from baseline to 1, 6, 12, and 24 months after the procedure.
In the modified intention-to-treat analysis of the REDUCE LAP-HF II trial, 621 patients were studied, with a median age of 72 years, and more than half were female. Of this group, 309 received the shunt treatment while 312 received the sham treatment.
Over 24 months, nearly all patients who received the shunt treatment had patent shunts (98%). Overall, implantation of the atrial shunt device led to improvements in various heart measurements compared with the sham treatment, such as reducing both the left ventricle (LV) end-diastolic volume (mean difference, −5.65 mL; P < .001) and left atrial (LA) minimal volume (mean difference, −2.8 mL; P =.01). It also improved certain aspects of heart function, including LV systolic tissue Doppler velocity (mean difference, 0.69 cm/s; P <. 001) and LA emptying fraction (mean difference, 1.88 percentage units; P =.02) compared with sham treatment. However, the device also caused both the right atrium (RA) and right ventricle (RV) to enlarge without affecting pumping or pressure on the right side.
In the shunt arm only, responders had smaller increases in the following, compared with nonresponders:
- RV end-diastolic volume (mean difference, 5.71 mL vs 15.18 mL; interaction P = .01)
- RV end-systolic volume (mean difference, 1.58 mL vs 7.89 mL; interaction P = .002)
- RV/LV ratio (mean difference, 0.07 vs 0.20; interaction P < .001)
Responders had larger increases in transmitral A wave velocity, with a mean difference of 5.08 cm/s vs −1.97 cm/s for nonresponders (interaction P =.02). Overall, those who responded well to the shunt treatment showed less enlargement of the right side of the heart and better blood flow through certain heart vessels compared with those who didn't respond as well. According to the researchers, this suggests that the shunt treatment might help relieve pressure on the left side of the heart by redirecting blood flow through the lungs.
“Taken together, these results represent the largest and most comprehensive echocardiographic follow-up study to date, to our knowledge, in a pivotal HFpEF randomized clinical trial and offer insights into the long-term effects of the atrial shunt device in this patient population,” the researchers said.
References
- Cardiac shunt. Cleveland Clinic. Accessed April 15, 2024. https://my.clevelandclinic.org/health/diseases/23057-cardiac-shunt
- Patel RB, Silvestry FE, Komtebedde J, et al. Atrial shunt device effects on cardiac structure and function in heart failure with preserved ejection fraction: the REDUCE LAP-HF II randomized clinical trial. JAMA Cardiol. Published online April 17, 2024. doi:10.1001/jamacardio.2024.0520