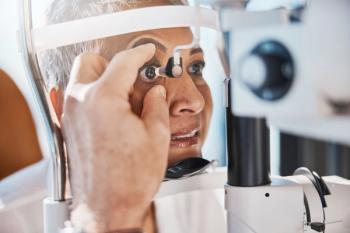
Considering Generic Vs Branded Therapy for Glaucoma
Experts debate the use of generic agents over branded therapy when managing patients with glaucoma.
Episodes in this series

Transcript:
Neil Minkoff, MD: The question I’m asking is when do you determine that a patient has failed a generic and needs to move to a branded agent, and then how do you pick the branded agent given that there are these new classes of drugs?
Terri-Diann Pickering, MD: If we start with a generic, I typically will have the patient come back in 2 to 3 weeks and recheck their intraocular pressure and look for certain percentage decrease in pressure, at least anywhere between 20% to 30%. If they respond, great, we continue treatment. If they don’t respond, then we can try a generic in a different class or we can then move on to a branded agent and make the appeal.
Neil Minkoff, MD: I’m going to keep pushing, but do you find an appeal is necessary? Many payors usually for most classes have an electronic system where if the patient has already been on the generic brand, it doesn’t necessarily require an appeal or extra work. Is that your experience? It doesn’t sound like it.
Terri-Diann Pickering, MD: No. I haven’t found that to be my experience.
Neil Minkoff, MD: OK. Dr Radcliffe?
Nathan Radcliffe, MD: My experience there is that after a drug has been on the market for 3 to 5 years, you start getting that type of process where maybe you hit a road bump or a simple PA [prior authorization] needs to be done. But almost like a box needs to be clicked type of PA that doesn’t require a lot of time. Early on though with a new therapy, it can be very difficult. The 1 thing I wanted to make is do we have an algorithm in my practice and I never get to follow it because my patients keep derailing me from my algorithm. A drop will sting 1 patient, it will make another patients’ eyes orange, red, another patient will have no adverse effects.
It is a master class in human variability to treat glaucoma because everyone will have something different going on. And that’s why we end up on all these different regimens, despite we’re just treating 1 disease with 1 goal, which is to lower the pressure. It really is patient driven that we end up kind of coming back to prescribe some obscure agent. I use pilocarpine [Salagen], which basically escaped FDA [Food and Drug Administration] approval, it’s such an old drug. We need all the tools we have, and we find ourselves reaching for them because patients, and their adverse effects, and reactions to these medications just push us in all these different directions.
Neil Minkoff, MD: Let me bring Dr Lopes back in and ask a question because 1 of the things we already have talked about is the disease prevalence increases with age, Medicare plans, Medicare Advantage plans, Part D plans, are probably the most important part of this. How does 1 like you look at tiering and out-of-patient cost in a Medicare plan for an aging population that might be facing blindness?
Maria Lopes, MD, MS: Yes, and also where you have available generics. We’re fortunate that in some mechanisms of action we have a plethora of generic options, and with some of the newer MOAs [mechanism of action] we do not have generic options. Where we have generic options, they’re usually available at very little cost to the patient. In my experience, where you have generic options, that’s where the new brands have a difficult time making it to preferred tier. And, if they’re covered, they’re usually in a nonpreferred tier, which means they’re covered. It’s just when patients try to access them at the pharmacy, they realize that it may be $100 and maybe a coinsurance, 30% coinsurance on a nonpreferred product, which patients simply can’t afford, especially if this is not the only drug they’re on. And many of these patients, this may be their 12th medication especially if they have multiple comorbidities. That’s the challenge.
Then you get into the medical exception, which is where the appeal comes in, as Dr Radcliffe mentioned. And the medical exception process is to justify what else [has] been tried and you’re trying to, essentially through an appeal process, help us understand that the drug that otherwise would be nonpreferred needs to be preferred because no other alternative exists. That is a barrier and that takes time away from providers. But we’re also reacting to the difference in the costs. There’s very little in the way of step management. It’s a difference in the tier, and then if patients can’t afford it, then this medical exception kicks in.
The other reason why something may not be covered is if it simply hasn’t been reviewed yet. And we have what’s called a moratorium on new drugs, new classes where initially for a period of sometimes 6 months, or in Medicare until the new year kicks in, and there’s now a new formulary in which products may not be readily available because they haven’t been reviewed, they’re not on formulary. And despite feeling that it’s appropriate, again you’d have to go through a medical exception process to help us understand the need to cover something that is higher cost.
Neil Minkoff, MD: I would love to get Dr Stephens to weigh in on the same question and then I have some other thoughts or questions about how drugs are used or switched. But I want to make sure that we’re getting Dr Stephens’s input on the formulary considerations especially in Medicare.
Kevin Stephens, Sr., MD: Again, let me go to the back end of the question first and then go backwards. The Medicaid population is totally different and that’s state driven, and typically the formulary is based on the state in that budget. The second one is that you have a commercial insurance, and the commercial insurance is interesting in that many times the cost of the plan is passed on to the employer. And when we have an employer, they have to look and they determine, we do some type of analytic, predictive model until we can tell what their disease burden is, and we price their premiums based upon the employee pool. And that’s a much more difficult population to manage because again, the employer is looking at what are we paying for and how much can we afford to pay. That’s a second problem in this whole picture, that we have different plans. We have Medicaid, commercial, and we have Medicare and we have different utilization management strategies and so forth.
The other comment I wanted to make though is that 1 underused thing that we have is a peer-to-peer process. And many times, we can get informal consideration, you can ask to speak to a reviewing physician. And when you talk to the reviewing physician, the medical director, you can say, “Look, here’s our problem. We tried on the generic. They’re allergic to sulfa. They have asthma. They have this, that, and the other, and this is my only option left.”
And, many times, you can avoid having to go through the appellate process and going through appeal by just doing a peer to peer and the medical director reviewing based upon the clinical diagnosis. Because many times our view to what’s going on with the patient is limited in many respects to what you fill out in the form, and you fax it or email it or however you send it to us. And many times, even the medical record is not as complete, and that’s why it’s important that we have these unusual, extraordinary cases that you should take advantage of that peer-to-peer process.
Transcript edited for clarity.
Newsletter
Stay ahead of policy, cost, and value—subscribe to AJMC for expert insights at the intersection of clinical care and health economics.