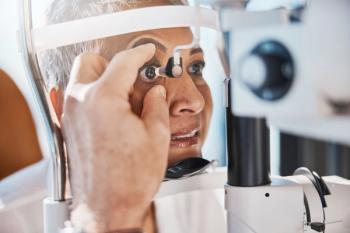
Glaucoma: Considering MIGS and Other Channel Procedures
Expert panelists review the use of MIGS and other channel procedures in patients with glaucoma.
Episodes in this series

Transcript:
Neil Minkoff, MD: What about something newer like MIGS [minimally invasive glaucoma surgery] therapy or other channel procedures? Where does that fit in compared to the more conventional, traditional procedures in terms of patient population or whom you’re picking for those types of therapies?
Terri-Diann Pickering, MD: MIGS is a move in the right direction because many of the MIGS procedures are done internally, so you don’t have to be worried about failure because the conjunctiva scars. You also don’t have to worry about long-term negative effects that can cause blindness in some cases, effects like infection, endophthalmitis, erosion of big implants that are put on the surface, bleb leaks, or chronic tearing, ocular surface disease from implants, and double vision. In general, we position the MIGS after or while a patient is on maximum medical therapy and they’ve also had laser trabeculoplasty, but before we would do a more invasive procedure, such as a trabeculectomy or a tube shunt implant.
Neil Minkoff, MD: Dr Radcliffe?
Nathan Radcliffe, MD: We had something nice recently. One of the trabecular microbypass stents, the Hydrus, has 5-year data. They showed this unique thing where compared to cataract surgery alone, patients who got a Hydrus, at 5 years were not going on to get the tubes and the trabeculectomies and the high morbidity glaucoma surgeries. Those surgeries, which I do all the time, they’re a negative life event for a patient to have to have invasive serious glaucoma surgery. There’s always a quality-of-life problem after. MIGS shows that even if you treat the cataract-only patient to the same pressure, the patient who got the MIGS will not only be on fewer drops 5 years out, but they’ll end up not having a surgery.
Then they just showed recently, they’ll have less visual field progression to boot, even with the same pressures treated medically. You’re seeing that doing these MIGS procedures, restoring physiologic outflow, treating the disease at its site along with cataract surgery will have benefits 5 years later to the patients, their quality of life. I assume there’s going to be some cost efficacy that comes in, but 5 years is a long time into the future, isn’t it? We’re all sort of thinking along that way, and I know that can be a challenge for payers to think that long term, given how things work.
Transcript edited for clarity.
Newsletter
Stay ahead of policy, cost, and value—subscribe to AJMC for expert insights at the intersection of clinical care and health economics.